QUIZ SECTION
Multiple Oral White Papules in a 3-year-old Girl: A Quiz
Jeanne BETTON1, Thibault KERVARREC2, Thomas DIDIER3, Catherine GAUDY-GRAFFIN4,5, Mahtab SAMIMI6 and Sophie LEDUCQ1,5,6*
1Unit of Pediatric Dermatology, Reference Center for Rare Diseases and Vascular Malformations (MAGEC), University Hospital Center of Tours, Tours, France, 2Department of Pathology, University Hospital Center of Tours, Tours, France, 3Department of Oral and maxillofacial Surgery, University Hospital Center of Tours, Tours, France, 4Department of Bacteriology, Virology and Hospital Hygiene, University Hospital Center of Tours, Tours, France, 5University of Tours, University of Nantes, INSERM 1246-SPHERE, Tours, France, and 6Department of Adult Dermatology, University Hospital Center of Tours, Tours, France. *Email: sophie.leducq@univ-tours.fr
Citation: Acta Derm Venereol 2026; 106: adv-2025-0086. DOI: https://doi.org/10.2340/actadv.v106.adv-2025-0086.
Copyright: © 2026 The Author(s). Published by MJS Publishing, on behalf of the Society for Publication of Acta Dermato-Venereologica. This is an Open Access article distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (https://creativecommons.org/licenses/by-nc/4.0/).
Submitted: Accepted after revision:
Published: Feb 09, 2026.
Competing interests and funding:
We report the case of a 3-year-old girl with no significant personal or family medical history who presented to the dermatology department with oral lesions evolving over 4 months. The lesions had progressively extended, leading to moderate discomfort, particularly during eating. Clinical examination revealed whitish, verrucous papules located on the inner cheeks, mucosal side of the lips and labial commissures (Fig. 1a). A full skin examination revealed no associated abnormalities. Initial laboratory testing, including complete blood count, serum protein electrophoresis, HIV serology, serum electrolytes and quantitative immunoglobulin levels, revealed no significant abnormalities. Skin biopsy showed epithelial acanthosis associated with viral cytopathic effects, including koilocytotic atypia within the spinous layer, characterized by hyperchromatic nuclei with perinuclear clear halos and binucleation, suggesting papillomavirus infection (Fig. 1b).
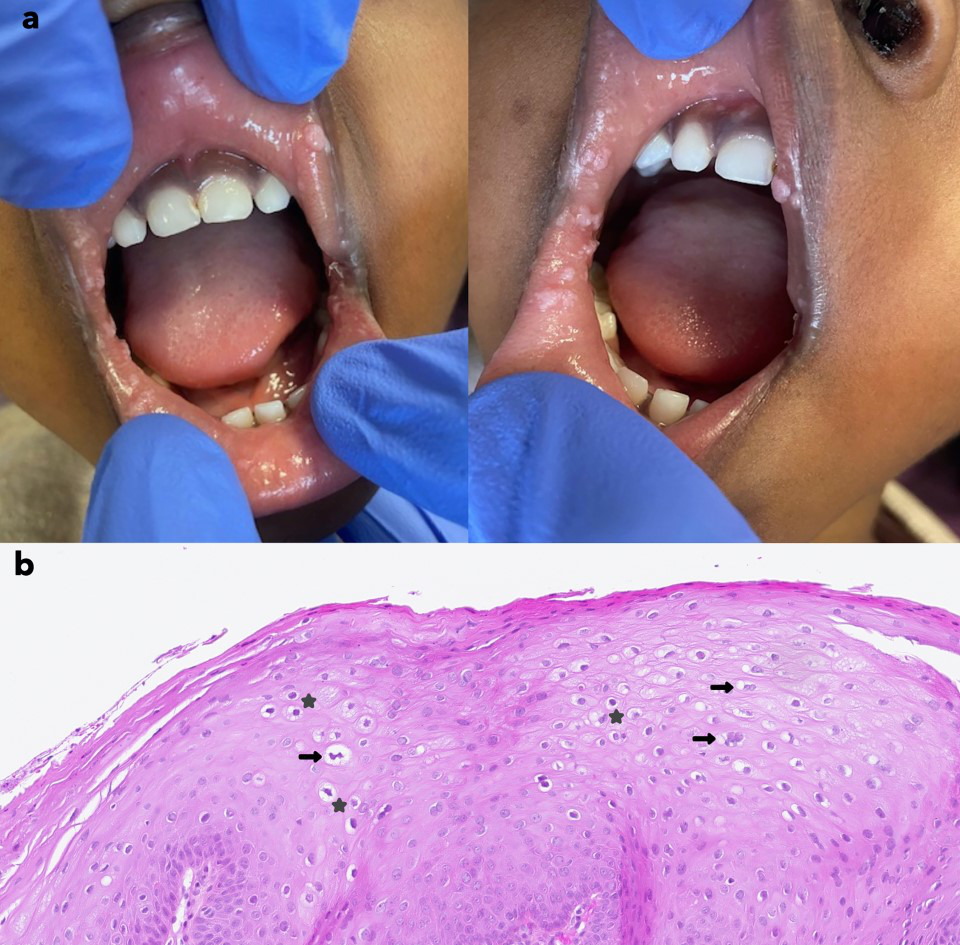
Fig. 1. (a) Multiple white papules on the oral mucosa of a 3-year-old girl. (b) Histology of skin biopsy showing a well-organized acanthotic squamous epithelium with focal parakeratosis. Presence of viral cytopathic effects within the spinous layer: koilocytic atypia with dark, smudged nuclei and perinuclear clear halos (stars), as well as binucleation (arrows) (haematoxylin-eosin stain, 400x).
What is your diagnosis?
1: Condyloma acuminatum
2: White sponge naevus
3: Focal epithelial hyperplasia
4: Cowden’s syndrome
See next page for answer.
ANSWERS TO QUIZ
Multiple Oral White Papules in a 3-year-old Girl: A Commentary
Diagnosis: Focal epithelial hyperplasia
The clinical presentation of our young patient highly suggested focal epithelial hyperplasia (FEH). PCR analysis performed on the skin biopsy revealed the presence of human papillomavirus 32 (HPV-32). The diagnosis of FEH was confirmed on considering clinical and histology findings (cytopathogenic changes) and PCR analysis (detection of HPV-32). The absence of cutaneous or extracutaneous involvement, along with normal blood findings, further supported the benign and localized nature of this condition.
FEH, also known as Heck’s disease, is a benign condition of the oral mucosa, mostly observed in young individuals. The mean age of affected patients is 23 years, with a male-to-female ratio of 3/4 (1). This pathology seems to preferentially affect certain ethnic groups, particularly Native Americans, Inuit and other indigenous populations (2).
The disease manifests as smooth-surfaced papules localized on the oral mucosa, affecting the lips, the inner cheeks, the tongue and occasionally the palate. The lesions are often asymptomatic and may spontaneously regress without sequelae. However, in some cases, they can persist and cause discomfort, functional or aesthetic, as observed in our case. In such situations, several therapeutic options can be considered, including surgical excision, laser treatment (CO2, diode), topical therapies (imiquimod, interferon-β) or photodynamic therapy (3, 4, 5). However, these treatments can be invasive, painful and may lead to adverse effects and, therefore, be poorly tolerated, particularly in the paediatric population. As a result, a conservative approach with therapeutic abstention and regular clinical monitoring is often preferred. For our patient, the latter approach was retained, and lesions spontaneously regressed within 9 months.
The aetiology of this condition is linked to infection with specific subtypes of HPV, particularly low-risk types 13 and 32, which are the most frequently identified in Heck’s disease (6). Nevertheless, other HPV subtypes have been identified, including high-risk types such as HPV-16, -18 and -31, as well as intermediate-risk types (7). A genetic predisposition has been suggested, notably via an association with the HLA-DR4 allele (8).
The diagnosis of FEH is based on clinical and histopathologic findings, although PCR can be useful for aetiological confirmation, particularly in identifying the specific HPV subtype involved.
This case contributes to a better characterization of this rare entity, especially in children, and highlights the importance of including it in the differential diagnosis of oral papillomatous lesions such as squamous cell papilloma, condyloma, Cowden’s disease, white sponge nevus or even verrucous carcinoma.
REFERENCES
- Sethi S, Ali A, Ju X, Antonsson A, Logan R, Jamieson L. An update on Heck’s disease-a systematic review. J Public Health (Oxf) 2022; 44: 269–285. https://doi.org/10.1093/pubmed/fdaa256
- Conde-Ferráez L, González-Losa MDR. Multifocal epithelial hyperplasia: an understudied infectious disease affecting ethnic groups. A mini review. Front Cell Infect Microbiol 2024; 14: 1420298. https://doi.org/10.3389/fcimb.2024.1420298
- Nallanchakrava S, Sreebala N, Basavaraj Sindgi F. Laser excision of focal epithelial hyperplasia (Heck’s Disease): a rare case report. Int J Clin Pediatr Dent 2018; 11: 526–528. https://doi.org/10.5005/jp-journals-10005-1569
- Yasar S, Mansur AT, Serdar ZA, Goktay F, Aslan C. Treatment of focal epithelial hyperplasia with topical imiquimod: report of three cases. Pediatr Dermatol 2009; 26: 465–468. https://doi.org/10.1111/j.1525-1470.2009.00954.x
- Tian X, Li Z, Dan H, Zeng X, Chen Q, Wang J. Photodynamic therapy in focal epithelial hyperplasia. Photodiagnosis Photodyn Ther 2023; 44: 103757. https://doi.org/10.1016/j.pdpdt.2023.103757
- Henke R, Guérin‐Reverchon I, Milde‐Langosch K, Koppang HS, Löning T. In situ detection of human papillomavirus types 13 and 32 in focal epithelial hyperplasia of the oral mucosa. J Oral Pathology Medicine 1989; 18: 419–421. https://doi.org/10.1111/j.1600-0714.1989.tb01575.x
- Jiménez Aguilar SM, Rodríguez DL, Muñoz Estrada VF, Cázarez Salazar SG, Velarde Félix JS, Méndez Martínez RS. Great diversity of oncogenic human papillomaviruses is revealed in an outbreak of multifocal epithelial hyperplasia. J Am Acad Dermatol 2023; 88: 1115–1117. https://doi.org/10.1016/j.jaad.2019.12.041
- García-Corona C, Vega-Memije E, Mosqueda-Taylor A, Yamamoto-Furusho JK, Rodríguez-Carreón AA, Ruiz-Morales JA, et al. Association of HLA-DR4 (DRB1*0404) with human papillomavirus infection in patients with focal epithelial hyperplasia. Arch Dermatol 2004; 140: 1227–1231. https://doi.org/10.1001/archderm.140.10.1227