SHORT COMMUNICATION
Is Staphylococcus epidermidis Involved in the Etiopathogenesis of Pitted Keratolysis?
Stefano VERALDI1* , Rossana SCHIANCHI2, Italo Francesco AROMOLO3
, Rossana SCHIANCHI2, Italo Francesco AROMOLO3 and Gianluca NAZZARO3
and Gianluca NAZZARO3
1Dermatological Centre in Milan, Milan, Italy, 2European Institute of Dermatology, Milan, Italy, and 3Department of Pathophysiology and Transplantation, Università degli Studi di Milano, Milan, Italy. *Email: stefano.veraldi@dcim.it
Citation: Acta Derm Venereol 2026; 106: adv-2025-0136. DOI: https://doi.org/10.2340/actadv.v106.adv-2025-0136.
Copyright: © 2026 The Author(s). Published by MJS Publishing, on behalf of the Society for Publication of Acta Dermato-Venereologica. This is an Open Access article distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (https://creativecommons.org/licenses/by-nc/4.0/).
Submitted: Oct 29, 2025. Accepted after revision: Feb 10, 2026.
Published: Mar 2, 2026.
Competing interests and funding: The authors have no conflicts of interest to declare.
The authors received no funding for this work.
Anonymized data will be shared upon reasonable request from any qualified investigator for purposes of replicating procedures and results.
In accordance with the guidelines of our institution's ethics committee, and given the nature of the study, formal approval was not required.
Written informed consent was obtained from the patient included in the study, regarding also the publication of the photos.
Pitted keratolysis (PK) is a superficial bacterial infection involving almost exclusively the soles. It is more common in tropical and subtropical countries, and in subjects who wear occlusive shoes for long periods. The most important risk factor is hyperhidrosis. PK is characterized by small, isolated or confluent, crateriform, noninflammatory pits. Maceration and bad smell are common (1). We recently published the case of a 37-year-old Caucasian man with PK in whom, for the first time, bacteriological examinations were positive for Staphylococcus aureus and S. epidermidis (1). After this case, we observed another patient with the same bacteriological results.
CASE REPORT
A 46-year-old Caucasian man was admitted with a clinical diagnosis of PK. The patient stated that he was in good general health and that he was not in therapy with systemic drugs. He worked as a mason and wore occlusive shoes for 8 h a day. He also stated that the dermatitis appeared 8 months before and that it was unsuccessfully treated with antiperspirants, zinc oxide, amikacin and gentamicin. Dermatological examination showed the presence of numerous confluent, crateriform, noninflammatory, macerated and malodorous pits located on the forefeet (Fig. 1). General physical examination was normal. Laboratory tests were within normal limits. Cytological examinations revealed the presence of numerous Gram-positive, coccoid-shaped bacteria. Swabs (flocked Copan, with eSwab technology) of some lesions were made. Transport swabs (in eSwab liquid medium, with 1 mL Amies liquid transport medium and probe with flocked nylon fibre tip) were used. Culture media used were 5% sheep blood agar (incubation for 24–48 h), MacConkey agar (incubation at 35–37°C for 24 h), mannitol salt agar (incubation at 35–37°C for 24 h) and Sabouraud dextrose agar (incubation at 32°C for 5 days). Bacteriological cultures were positive for S. aureus and S. epidermidis. A semi-quantitative assessment of bacterial load was used. S. epidermidis and S.aureus were identified by mass spectrometry (matrix assisted laser desorption ionization timer-of-flight [MALDI-TOF]), performed on samples obtained from cultures.
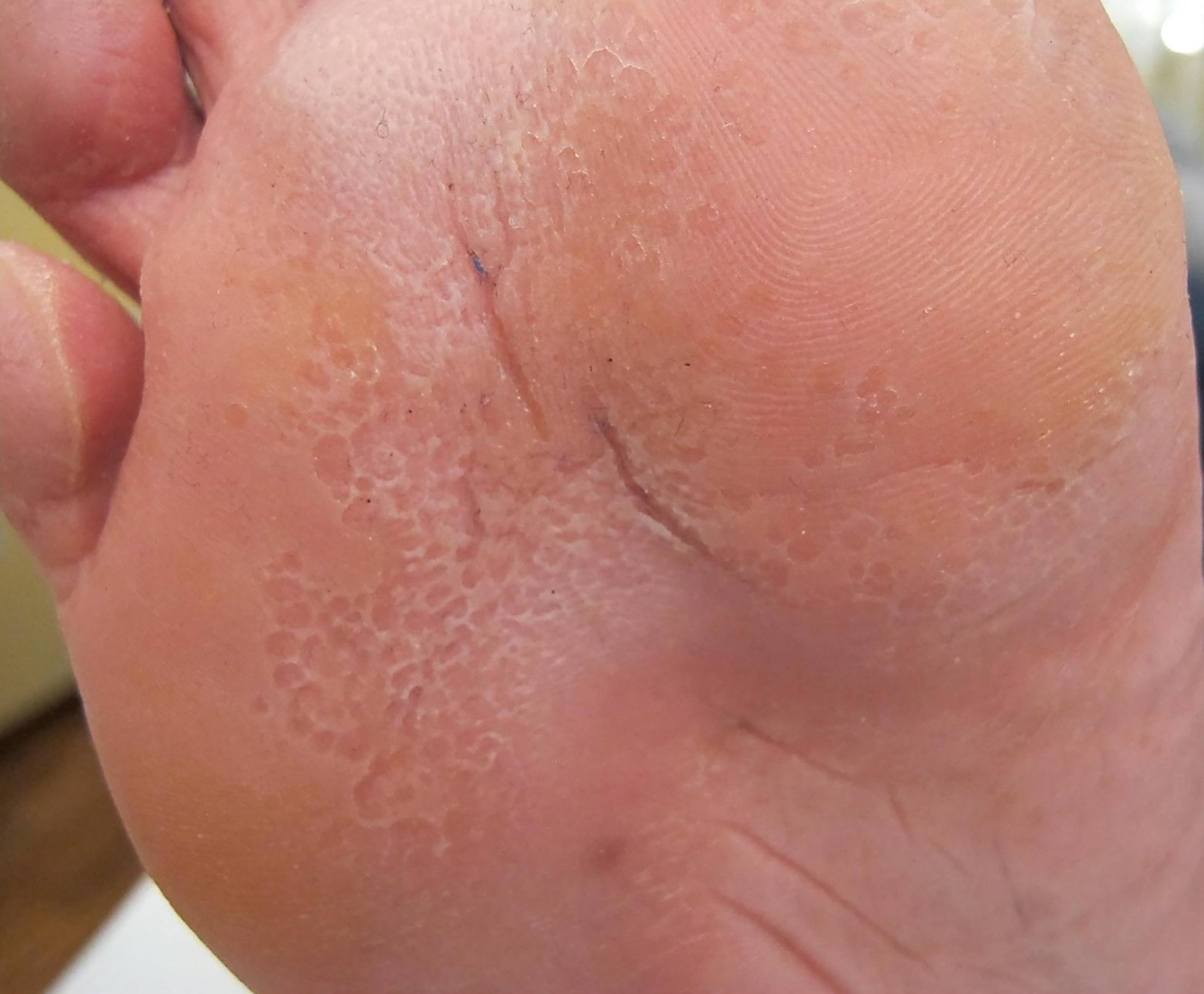
Fig. 1. Confluent, crateriform, noninflammatory, macerated pits located on a forefoot: pitted keratolysis.
DISCUSSION
Several bacteria were considered as possible aetiological agents of PK. Dermatophilus congolensis releases keratinases which are able to degrade keratin (2, 3, 4, 5, 6). Other possible involved bacteria are Microcossus sedentarius (PK was produced experimentally in a volunteer by applying this bacterium under occlusive dressing on a heel) (7), Kytococcus sedentarius (the novel name of M. sedentarius), which produces two proteases, P1 and P2 (8), and Bacillus thuringiensis (9). Coccoid and diphtheroid bacteria (10, 11) and Corynebacterium sp. (12, 13, 14, 15) were also isolated. These bacteria are both inter- and intracellular (10, 11). In summary, most authors observed the growth of Gram-positive, pleomorphic, aerobic bacteria (12). However, in the study by Nordstrom et al., bacteriological examinations were positive for Gram-negative bacteria, diphtheroids, Corynebacterium minutissimum, Brevibacterium sp., S. aureus and coagulase-negative staphylococci (7). In our patient, and in the patient we previously reported (1), bacteriological examinations, including culture and MALDI-TOF, were positive for S. aureus and S. epidermidis, i.e., two Gram-positive, catalase-positive, coagulase-negative bacteria. As S. epidermidis is a ubiquitous commensal on the skin, it is difficult to explain its potential etiopathogenetic role in PK. Further studies are therefore necessary. However, our results and literature review confirm that PK can be caused by different bacteria.
REFERENCES
- Veraldi S, Schianchi R, Aromolo IF, Nazzaro G. Treatment of chronic-relapsing pitted keratolysis with glycopyrronium bromide cream: case report. Case Rep Dermatol 2025; 17: 9–13. https://doi.org/10.1159/000542484
- Rubel LR. Pitted keratolysis and Dermatophilus congolensis. Arch Dermatol 1972; 105: 584–586.
- Woodgyer AJ, Baxter M, Rush‐Munro FM, Brown J, Kaplan W. Isolation of Dermatophilus congolensis from two New Zealand cases of pitted keratolysis. Australas J Dermatol 1985; 26: 29–35. https://doi.org/10.1111/j.1440-0960.1985.tb01811.x
- Gillum RL, Qadri SM, Al-Ahdal MN, Connor DH, Strano AJ. Pitted keratolysis: a manifestation of human dermatophilosis. Dermatologica 1988; 177: 305–308. https://doi.org/10.1159/000248584
- Hänel H, Kalisch J, Keil M, Marsch WC, Buslau M. Quantification of keratinolytic activity from Dermatophilus congolensis. Med Microbiol Immunol 1991; 180: 45–51. https://doi.org/10.1007/BF00191700
- Da Fonseca FA. Pitted keratolysis – The role of Dermatophilus congolensis. J Eur Acad Dermatol Venereol 1996: S134.
- Nordstrom KM, McGinley KJ, Cappiello L, Zechman JM, Leyden JJ. Pitted keratolysis. The role of Micrococcus sedentarius. Arch Dermatol 1987; 123: 1320–1325. https://doi.org/10.1001/archderm.123.10.1320
- Longshaw CM, Wright JD, Farrell AM, Holland KT. Kytococcus sedentarius, the organism associated with pitted keratolysis, produces two keratin-degrading enzymes. J Appl Microbiol 2002; 93: 810–816. https://doi.org/10.1046/j.1365-2672.2002.01742.x
- Schneider G, Schweitzer B, Kovács T. Bacillus thuringiensis: a causative agent of pitted keratolysis. Australas J Dermatol 2021; 62: e609–e611. https://doi.org/10.1111/ajd.13718
- Tilgen W. Pitted keratolysis (keratolysis plantare sulcatum). Ultrastructural study. J Cutan Pathol 1979; 6: 18–30. https://doi.org/10.1111/j.1600-0560.1979.tb00302.x
- Wohlrab J, Rohrbach D, Marsch WC. Keratolysis sulcata (pitted keratolysis): clinical symptoms with different histological correlates. Br J Dermatol 2000; 143: 1348–1349. https://doi.org/10.1046/j.1365-2133.2000.03934.x
- Shelley WB, Shelley ED. Coexistent erythrasma, trichomycosis axillaris, and pitted keratolysis: an overlooked corynebacterial triad? J Am Acad Dermatol 1982; 7: 752–757. https://doi.org/10.1016/s0190-9622(82)80158-8
- Conti Díaz IA, Peluffo IC, Calegari L, Sanabria D, Viegas MC. Queratólisis en hoyuelos (pitted keratolysis) a forma hiperqueratósica y aislamiento del agente etiológico: Corynebacterium sp. Med Cutan Ibero Lat Am 1987; 15: 157–160.
- Rho NK, Kim BJ. A corynebacterial triad: Prevalence of erythrasma and trichomycosis axillaris in soldiers with pitted keratolysis. J Am Acad Dermatol 2008; 58: S57–8. https://doi.org/10.1016/j.jaad.2006.05.054
- Zaias N. Pitted and ringed keratolysis. A review and update. J Am Acad Dermatol 1982; 7: 787–791. https://doi.org/10.1016/s0190-9622(82)70162-8