Sudden Onset of Unilateral Facial Paralysis with Ear Pruritus: A Quiz
Aleksandra A. Stefaniak, Klaudia Knecht, Łukasz Matusiak and Jacek C. Szepietowski*
Department of Dermatology, Venereology and Allergology, Wroclaw Medical University, ul. Chałubińskiego 1, PL-50-368 Wrocław, Poland. *E-mail: jacek.szepietowski@umed.wroc.pl
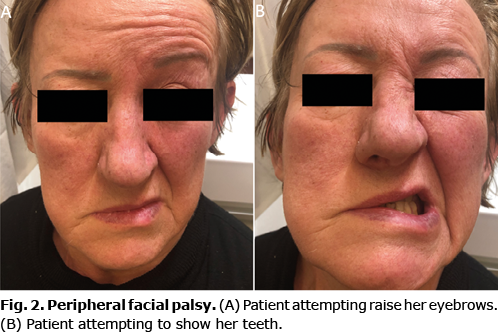
A 60-year-old woman presented with right facial muscle paralysis together with otalgia and local pruritus of the affected ear. In addition, she developed vertigo, tingling and numbness of the tongue, nausea and vomiting. The patient reported a continuous fever, up to 38°C. Ear, nose and throat assessment revealed patent external auditory meatus and vesicles with serous content. There were no significant alterations in the tympanic membrane and auricles tenderness while pulling. In the oral cavity, serous vesicles were visible on the hard palate and on the right side of the tongue (Fig. 1A). Moreover, the patient reported left-sided horizontal-rotary nystagmus. Her pupils were equal in size, round and responding correctly to light. Upon admission to the dermatological department, a detailed physical examination revealed numerous erosions in the oral cavity, swelling of the ear and scabs on the erythematous base of the right concha (Fig. 1B). Paralysis of the right facial muscles was noted (Fig. 2). On attempting to close her eyes, an eyelid gap occurred due to incomplete eye closure at effort. This was accompanied by drooping of the corner of the mouth. Meningeal symptoms were negative, and no other peripheral sensory impairment was observed. Computer tomography of the head did not reveal any neurological changes.

What is your diagnosis? See next page for answer.
Sudden Onset of Unilateral Facial Paralysis with Ear Pruritus: A Commentary
Acta Derm Venereol 2022; 102: adv00675.
DOI: 10.2340/actadv.v102.756
Diagnosis: Ramsay Hunt syndrome
Ramsay Hunt syndrome is a rare disorder attributed to reactivation of pre-existing varicella zoster virus (VZV) infection. VZV is an exclusively human virus classified to the Herpesviridae family. After initial infection, the virus establishes latency in the cranial nerves and dorsal root ganglia (1, 2). It may become reactivated as a herpes zoster, typically appearing as erythematous vesicular lesions clustered within a single dermatome. On the whole, Ramsay Hunt syndrome is a rare type of herpes zoster attributed to dysfunction of the geniculate ganglion (1–3) with an annual incidence estimated at 5 in 100,000 with a slight female predominance (4). It results from involvement of the geniculate ganglion of the VII cranial nerve. The syndrome consists of acute ipsilateral facial paralysis, exquisite otalgia and erythematous vesicular rash near the ear, mastoid and external auditory meatus (5). At onset, it might be indistinguishable from Bell’s palsy, especially when facial paralysis occurs prior to the appearance of the vesicular lesions. Some researchers suggest that Bell’s palsy without visible skin lesions may also be the result of VZV reactivation; therefore, antiviral therapy should always be considered (6). Dizziness, vertigo with nystagmus towards the healthy ear, tinnitus and disturbances in taste perception may also occur (7). For diagnosis, it is important to perform computer tomography (CT) of the head without contrast, to exclude neurological origin of the symptoms. The vestibulocochlear nerve (VIII cranial nerve) can also become affected due to the adjacent location. For this reason, the following symptoms may appear: tinnitus, nausea, vomiting and partial, or even complete, hearing loss.
Diagnosis of Ramsay Hunt syndrome is usually based on clinical features and the patient’s history. Multinucleated giant cells can be demonstrated in Tzanck smear from material scraped from the base of vesicular lesions and stained with haematoxylin and eosin (H&E) or Giemsa stain. In Ramsay Hunt syndrome, a 4-fold increase in anti-VZV antibodies or the presence of VZV DNA can be detected in the saliva, tears or blood monocytes (8, 9).
The major benefits of antiviral therapy in patients with Ramsay Hunt syndrome are reductions in duration, severity of pain, extent of skin lesions in the primary dermatomes and spread of the disorder elsewhere in the body. Antiviral therapy combined with steroids can reduce debilitating complications, such as post-herpetic neuralgia. The current patient was treated with intravenous aciclovir (500 mg, 3 times per day) and prednisone (60 mg at onset, followed by gradual reduction). In addition, vitamin B (B1, B6, B12) supplementation was introduced with intensive physiotherapy. This therapy has been shown to have enhanced outcomes compared with antiviral drugs in monotherapy (10). In general, the treatment should be initiated within 72 h of onset. The correct dosage is established according to the House-Brackmann grading system (11), which is a widely used facial nerve dysfunction grading scale governed by the intensity of the pain. It is important to mitigate sleep deprivation caused by the pain. Long-acting opioids and tricyclic antidepressants have proved effective, as well as a single dose of 900 mg gabapentin (12–15). In the case of a positive Schirmer’s test, artificial tears should be prescribed to avoid corneal abrasion. If pain management remains inadequate, local anaesthetic nerve blocks should be performed (13).
REFERENCES
- Zerboni L, Sen N, Oliver SL. Molecular mechanisms of varicella zoster virus pathogenesis. Nat Rev Microbiol 2014; 12: 197–210.
- Al-Turab M, Chehadeh W. Varicella infection in the Middle East: prevalence, complications, and vaccination. J Res Med Sci 2018; 23: 19.
- Kennedy PGE. Varicella-zoster virus latency in human ganglia. Rev Med Virol 2002; 12: 327–334.
- Yawn BP, Gilden D. The global epidemiology of herpes zoster. Neurology 2013; 81: 928–930.
- Ostwal S, Salins N, Deodhar J, Muckaden MA. Management of Ramsay Hunt syndrome in an acute palliative care setting. Indian J Palliat Care 2015; 21: 79–81.
- Furuta Y, Aizawa H, Ohtani F, Sawa H, Fukuda S. Varicella-zoster virus DNA level and facial paralysis in Ramsay Hunt syndrome. Ann Otol Rhinol Laryngol 2004; 113: 700–705.
- Oxman MN. Clinical manifestations of herpes zoster. In: Arvin AM, Gershon AA, editors. Varicella-zoster virus: virology and clinical management. Cambridge, UK: Cambridge University Press 2000: 246.
- Kim D, Bhimani M. Ramsay Hunt syndrome presenting as simple otitis externa. CJEM 2008; 10: 247–250.
- Sweeney C, Gilden D. Ramsay Hunt syndrome. J Neurol Psych 2001; 71: 149–154.
- Uscategui T, Doree C, Chamberlain IJ, Burton MJ. Corticosteroids as adjuvant to antiviral treatment in Ramsay Hunt syndrome (herpes zoster oticus with facial palsy) in adults. Cochrane Database Syst Rev 2008; 16: CD006852.
- Coulson S, Croxson GR, Adams R, Oey V. Prognostic factors in herpes zoster oticus (Ramsay Hunt syndrome). Otol Neurotol 201; 32: 1025–1030.
- Dworkin RH, Johnson RW, Breuer J, Gnann JW, Levin MJ, Backonja M, et al. Recommendations for the management of herpes zoster. Clin Infect Dis 2007; 44: S1–S26.
- Berry JD, Petersen KL. A single dose of gabapentin reduces acute pain and allodynia in patients with herpes zoster. Neurology 2005; 65: 444–447.
- Furuta Y, Aizawa H, Sawa H, Ohtani F, Fukuda S. Varicella-zoster virus dna level and facial paralysis in Ramsay Hunt syndrome. Ann Otol Rhinol Laryngol 2004; 113: 700–705.
- Werner RN, Nikkels AF, Marinović B, Schäfer M, Czarnecka-Operacz M, Agius AM, et al. European consensus-based (S2k) guideline on the management of herpes zoster – guided by the European Dermatology Forum (EDF) in cooperation with the European Academy of Dermatology and Venereology (EADV), Part 2: Treatment. J Eur Acad Dermatol Venereol 2017; 31: 20–29.

