QUIZ SECTION
A Reddish Nodule on the Scalp: A Quiz
Renqiong CHEN1,2*, Qing LUO1,2*, Guangquan JI3,4 and Hong REN1,2
1Department of Dermatology, 2Department of Dermatology, 3Department of Technology, Affiliated Lianyungang Hospital of Xuzhou Medical University, Lianyungang, China, 4Department of Technology, The First Affiliated Hospital of Kangda College of Nanjing Medical University. *E-mails: chenrenqiong718@126.com; luoqing0401@126.com.
Citation: Acta Derm Venereol 2023; 103: adv9596. DOI https://doi.org/10.2340/actadv.v103.9596.
Copyright: © Published by Medical Journals Sweden, on behalf of the Society for Publication of Acta Dermato-Venereologica. This is an Open Access article distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (https://creativecommons.org/licenses/by-nc/4.0/)
Published: May 29, 2023
Competing interests and funding: The authors have no conflicts of interest to declare.
A 47-year-old woman presented with an asymptomatic nodule on her head. She first noticed the lesion approximately 1 year previously. Clinical examination revealed a slight reddish surface-coloured, elastic hard nodule, measuring approximately 1 cm on her scalp (Fig. 1). Regional lymph nodes were not involved. The skin lesion was completely resected under local anaesthesia and the margins were free of tumour. Microscopic examination revealed numerous small tumour cell islands floating in a mucin lake in the dermis (Fig. 2). Immunohistochemistry showed positive staining for CK7, GATA3, ER, PR and Ki67, weakly positive staining for GCDFP-15 and P63 and negative staining for TTF-1, CK20, CDX-2 and HER2 (Fig. 2). Medical history and breast examination revealed nodules in both nipples. Histological examination revealed adenosis of the left breast with intraductal papilloma along with small focal ductal epithelial dysplasia, and adenosis of the right breast with focal ductal epithelial hyperplasia.
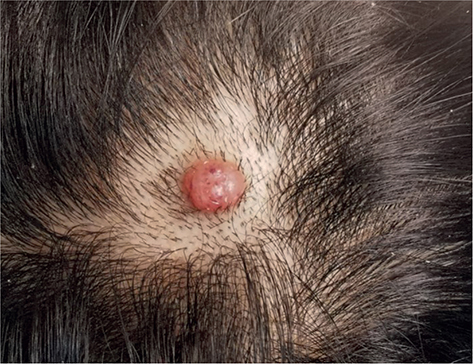
Fig. 1. Skin lesion on the scalp.
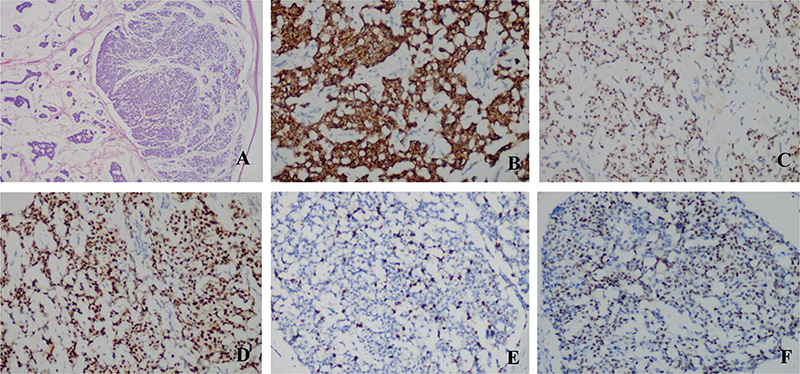
Fig. 2. A pathological slice of the nodule revealed pools of extracellular mucin with islands of tumour (haematoxylin and eosin (HE) staining: (A) 40×). Immunohistochemistry: (B–F: 200×). (B) CK7(+); (C) GATA3(+); (D) ER(+); (E) Ki67(+); (F) PR(+).
What is your diagnosis? See next page for answer.
ANSWERS TO QUIZ
A Reddish Nodule on the Scalp: A Commentary
Diagnosis: Primary cutaneous mucinous carcinoma
Primary cutaneous mucinous carcinoma (PCMC) was first described by Lennox et al. (1) and is a rare subtype of sweat gland tumour. Controversy about the apocrine or eccrine origins of this tumour exists, but most authors favour eccrine differentiation as the origin (2). PCMC is sometimes misdiagnosed as metastatic skin carcinoma, especially breast carcinoma or gastrointestinal carcinoma. Therefore, internal malignancies should be ruled out, since the subcutaneous lesion could represent a metastatic skin tumour. Immunohistochemically, metastatic mucinous carcinoma of gastrointestinal carcinoma is largely indicated if CK20 and CDX2 are stained in tumour cells (3, 4). Similar to previous studies (5, 6), the tumour cells in the current case were negative for CK20, TTF1 and CDX2. Thus, the possibility of a metastatic primary mucinous carcinoma of gastrointestinal carcinoma could be completely ruled out. However, immunohistochemistry showed positive staining for GATA3, ER and PR. Therefore, it was necessary to rule out breast carcinoma. A medical history and breast examination revealed nodules in the right and left nipples. Histological examinations revealed adenosis of the left breast with intraductal papilloma along with small focal ductal epithelial dysplasia, and adenosis of the right breast with focal ductal epithelial hyperplasia. Thus, breast carcinoma was ruled out. These findings therefore support a diagnosis of PCMC.
PCMC is a rare malignant skin adnexal neoplasm that commonly arises on the head, face and neck. It occurs more often in men than women, and appears most frequently between the ages of 50 and 70 years. Clinically, the lesion presents as a slow-growing, erythematous or grey-blue painless nodule (0.5–7 cm in diameter), which may be indurated or ulcerated (7). PCMC of the skin has a relatively good prognosis with lower rates of distant metastases (9.6%, commonly to regional lymph nodes), but local recurrence rate as high as 29.4% (8, 9). The recommended treatment includes surgical excision with a minimum of 10-mm margin (10). In this case, the skin lesion was completely resected under local anaesthesia and the margins were free of tumour. However, further follow-up of the patient is necessary for prompt detection of local recurrence of the lesion.
PCMC is a rare malignancy that can present as a benign skin lesion. Physicians should be aware of this tumour and be able to differentiate it from benign cystic or solid lesions.
ACKNOWLEDGEMENT
This study was supported by Lianyungang Science and Technology Development Project (SF2236).
REFERENCES
- Lennox B, Pearse AG, Richards HG. Mucin-secreting tumours of the skin with special reference to the so-called mixed-salivary tumour of the skin and its relation to hidradenoma. J Pathol Bacteriol 1952; 64: 865–880.
- Carson HJ, Gattuso P, Raslan WF, Reddy V. Mucinous carcinoma of the eyelid. An immunohistochemical study. Am J Dermatopathol 1995; 17: 494–498.
- Drew JE, Farquharson AJ, Mayer CD, Vase HF, Coates PJ, Steele RJ, et al. Predictive gene signatures: molecular markers distinguishing colon adenomatous polyp and carcinoma. PLoS One 2014; 9: e113071.
- Breiting L, Christensen L, Dahlstrøm K, Breiting V, Winther JF. Primary mucinous carcinoma of the skin: a population-based study. Int J Dermatol 2008; 47: 242–245.
- Miyata K, Go U, Oide T, Mitsuishi T. Primary cutaneous mucinous carcinoma of the abdomen. Ann Dermatol 2019; 31: 339–340.
- Robinson M, Kelly J, Biberdorf D, McAuley I. Primary cutaneous mucinous carcinoma of the penis. Can Urol Assoc J 2014; 8: E89–91.
- Kamalpour L, Brindise RT, Nodzenski M, Bach DQ, Veledar E, Alam M. Primary cutaneous mucinous carcinoma: a systematic review and meta-analysis of outcomes after surgery. JAMA Dermatol 2014; 150: 380–384.
- Scilletta A, Soma PF, Grasso G, Scilletta R, Pompili G, Tarico MS, et al. Primary cutaneous mucinous carcinoma of the cheek. Case report. G Chir 2011; 32: 323–325.
- Sudesh R, Siddique S, Pace L. Primary eyelid mucinous adenocarcinoma of eccrine origin. Ophthalmic Surg Lasers 1999; 30: 394–395.
- Abiola OO, Ano-Edward GH, Oluwumi OA, Lasisi ME. Primary cutaneous mucinous carcinoma of the scrotum: a rare tumor at a rare site – a case report and review of literature. Urol Ann 2020; 12: 83–86.