ORIGINAL REPORT
RESULTS FROM THE INTERNATIONAL SPINAL CORD INJURY COMMUNITY SURVEY: THE LIVED EXPERIENCE OF PEOPLE WITH SPINAL CORD INJURY IN SOUTH-EASTERN BRAZIL
Daniela Mitiyo Odagiri UTIYAMA1, MSc, Fábio Marcon ALFIERI2*, PhD, Vinícius Delgado RAMOS2, MSc and Linamara Rizzo BATTISTELLA2,3, PhD
From the 1Instituto de Medicina Fisica e Reabilitacao, Hospital das Clinicas HCFMUSP, Faculdade de Medicina, Universidade de Sao Paulo, Sao Paulo, SP, BR, 2Clinical Research Center, Instituto de Medicina Fisica e Reabilitacao, Hospital das Clinicas HCFMUSP, Faculdade de Medicina, Universidade de Sao Paulo, Sao Paulo, SP, BR and 3Faculdade de Medicina FMUSP, Universidade de Sao Paulo, Sao Paulo, SP, BR
Objective: The incidence of spinal cord injury in Brazil is increasing. It is important to understand more about how individuals are living with spinal cord injury.
Design: Cross-sectional, observational study of individuals with spinal cord injury in south-eastern Brazil.
Subjects: A questionnaire with 125 questions was applied to individuals diagnosed with spinal cord injury. Participants were recruited by survey team from 2 rehabilitation centres (both in south-eastern Brazil) that treat persons diagnosed with SCI. Personal characteristics, associated health conditions, quality of life, work status, environmental factors, and other functioning-related aspects were evaluated.
Results: A total of 201 individuals participated in the survey. Of these, 79% were male, mean age 44 years, 60% were considered paraplegic, and the major causes of impairment were firearm injuries and road traffic accidents. Spasticity was the most frequently reported health condition, followed by neuropathic pain. 50% of subjects did not report any difficulty with participation in activities of daily living. However, only approximately 10% of subjects returned to work after spinal trauma. Their quality of life is reported 44% as good.
Conclusion: Most people with spinal cord injury in south-eastern Brazil are male and paraplegic, health problems and spasticity is considered their most problematic health condition. Although they report having a good quality of life, they still encounter disabling environmental barriers that make their life more difficult, such as poor accessibility of public spaces, and only a small proportion (10%) returned to work after their injury. This study provides an initial overview of the lived experience of people with spinal cord injury in south-eastern Brazil and should serve as a starting point for future research on this population.
LAY ABSTRACT
The number of cases of spinal cord injury in Brazil is increasing. It is important to know more about how individuals are living with this condition. A questionnaire with 125 questions was applied to individuals diagnosed with spinal cord injury Participants were recruited by survey team from 2 rehabilitation centres (both in south-eastern Brazil) that treat persons diagnosed with SCI. Personal characteristics, associated health conditions, quality of life, work status, environmental factors, and other functioning-related aspects were evaluated. A total of 201 individuals participated in the survey. Of these, 79% were male, and the major causes of impairment were firearm injuries and road traffic accidents. Fifty percent of individuals did not report any difficulty performing activities of daily living. Although people with spinal cord injury reported having a good quality of life, they still encounter disabling environmental barriers that make their life more difficult. This study provides an initial overview of the lived experience of people with spinal cord injury in south-eastern Brazil and should serve as a starting point for future research on this population.
Key words: spinal cord injury; spinal cord injury characteristics; work; functioning; health conditions.
Citation: J Rehabil Med 2022: jrm00342. DOI: http://dx.doi.org/10.2340/jrm.v54.2157.
Copyright: © Published by Medical Journals Sweden, on behalf of the Foundation for Rehabilitation Information. This is an Open Access article distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (https://creativecommons.org/licenses/by-nc/4.0/)
Accepted: Sep 27, 2022; Epub ahead of print: Oct 18, 2022; Published: Nov 29, 2022
Correspondence address: Fabio Marcon Alfieri, Clinical Research Center, Institute of Physical Medicine and Rehabilitation, University of São Paulo School of Medicine, Rua Domingo de Soto 100, Vila Mariana, 04116-030 São Paulo, SP, Brazil. E-mail: fabioalfieri@usp.br
Competing interests and funding: The authors have no conflicts of interest to declare.
Spinal cord injury (SCI) is one of the most serious and devastating disabling events. SCI can result in severe motor, urinary, intestinal, and sexual dysfunction, among others, altering individuals’ autonomy, quality of life, overall satisfaction and lifestyle, in addition to affecting their participation in society (1, 2).
Despite inconsistencies in data on the incidence and prevalence of SCI, some recent estimates indicate that 250,000–500,000 people are affected by SCI yearly (1–4).
According to Singh et al. (2), the country with the highest prevalence of persons with SCI is the USA (906 people per million), with SCI affecting mostly males, and was due by injuries (road traffic accidents), followed by falls in the elderly population. This number has increased in recent years; in 1975 the prevalence of SCI was approximately 30 people per million in the USA (5). Better understanding of the prevalence of SCI enables healthcare systems to implement preventive strategies and allocate appropriate resources to manage the consequences of this condition.
According to Botelho et al. (6), the incidence of SCI in Brazil is 40 new cases per year per million inhabitants; approximately 6,000–8,000 new cases each year. Of these individuals, 80% are male, and 60% are in the age range 10–30 years (1, 7, 8).
In 2013, the International Perspectives on Spinal Cord Injury (IPSCI) report (3) summarized a large amount of evidence and indicated that persons with SCI had a higher risk of mortality and were at greater risk of developing physical and mental health conditions. In addition to the risk of premature mortality and morbidity, SCI has been associated with reduced participation in social and economic activities, resulting in higher social exclusion and unemployment rates compared with in the worldwide population.
The environmental barriers that hinder persons with SCI from participating fully in society and from maintaining an optimal standard of health contribute to this situation. Inadequate policy and service delivery, a lack of assistive products, inaccessible environments, negative attitudes towards people with disabilities and a lack of knowledge and skills among health professionals are examples of barriers that influence people’s daily lives and, ultimately, their health and quality of life (3, 4, 9, 10).
Health status and functioning play an important role in allowing persons with SCI to participate in daily life and social activities in general. Recent studies of persons with SCI, such as the International Spinal Cord Injury (InSCI) Community Survey (9) and the Swiss Spinal Cord Injury Cohort (SwiSCI) (10), use the components of the International Classification of Functioning, Disability and Health and Disability (ICF) (11) as a reference to collect data on this condition and identify the most appropriate approaches to manage impairments in body structures and functions and limitations in activities and social participation, as well as the personal and environmental factors surrounding persons living with SCI for longer (12) or shorter periods (13).
The InSCI survey was developed to describe the lived experience of persons with SCI in the participating countries and, in particular, to collect data on the functioning, health and well-being of these individuals.
The incidence of SCI in Brazil is increasing and there is a need to understand more about how individuals are living with this condition. Although there are studies providing epidemiological data (6, 7) and on some functioning aspects (11–13), no study has observed the issues reported by persons with SCI in relation to their lived experience after the injury in relation to health, accessibility barriers, quality of life, and work status. Therefore, the current study addresses issues that may contribute to setting new policies and practices, as well as providing evidence input for rehabilitation professionals treating persons with SCI. As such, the aim of this study is to provide data on persons with SCI, in south-eastern Brazil their personal characteristics, environmental factors, associated health conditions, quality of life, work status and other functioning-related aspects.
METHODS
This cross-sectional, observational study was approved by the Institutional Review Board of the University of Sao Paulo Medical School General Hospital, Sao Paulo, Brazil (registration number CAAE 97049118.8.0000.0068) in order to comply with the requirements of the Institutional Review Board, verbal consent was obtained from participants because there was the approval of the Institutional Review Board (IRB).
Participants were recruited from 2 rehabilitation centres that treat persons diagnosed with SCI; the Physical and Rehabilitation Medicine Institute (IMREA) of the University of Sao Paulo Medical School General Hospital and the Rio de Janeiro Rehabilitation Association (Portuguese acronym: AFR) in 2 neighbouring south-eastern states in Brazil: São Paulo and Rio de Janeiro, respectively.
At the Physical and Rehabilitation Medicine Institute (IMREA) of the University of Sao Paulo Medical School General Hospital, the survey team contacted every patient with SCI who had received care at any time during the 2 years (2017–2019) prior to the study. The sample of patients with SCI at the AFR was obtained for convenience. These subjects were those who were on treatment during the study period. All individuals were invited to take part and be interviewed to confirm if they met the eligibility criteria described below. All participants were able to be interviewed by phone or video call or to reach the evaluation site independently, and gave either written or verbal consent to participate in the study. The study team used a mixed approach towards questionnaire administration. When self-administration was not feasible, questionnaires were administered by an experienced member of the team via phone or video calls.
Survey participants
Study participants were of both sexes, aged 18 years and older, with a diagnosis of SCI and at least 3 months since injury onset, according to information published elsewhere (14). Persons with SCI resulting from congenital causes, spina bifida, neurodegenerative diseases (such as multiple sclerosis and amyotrophic lateral sclerosis), peripheral nerve injuries, first-time rehabilitation inpatients and individuals in acute care were excluded.
Survey questionnaire
The questionnaire (International Spinal Cord Injury Survey) was prepared by the InSCI survey team (3) and translated (by 2 independent translators) into Portuguese from English, incorporating necessary cross-cultural adaptations the questionnaire was tested questionary with 10 participants prior to starting the study (14). (The questionnaire is available from: https://www.revistas.usp.br/actafisiatrica/article/view/172051/162697). The questionnaire comprises 125 questions and takes 25–40 min to complete. It aims to explore the lived experience of persons with SCI, based on 47 ICF components covering health conditions, psychosocial factors, injury characteristics (e.g. self-reported severity, cause and date of onset), quality of life, health and physical well-being. The InSCI questionnaire included questions from a range of measures, as described below.
Regarding quality of life and mental health, the questionnaire builds on the Short Form (SF)-36 survey (15) and the Spinal Cord Injury Secondary Conditions Scale (16). Activity and participation were assessed mainly by questions from the World Health Organization (WHO) Model Disability Survey (MDS) (17), the Spinal Cord Independence Measure (18) and the Spinal Cord Injury Functional Index (19).
The assessment of integration and health at work involves questions regarding the work environment and accessibility. Environmental factors were evaluated mainly with the Nottwil Environmental Factors Inventory Short Form (20).
Relevant personal factors were measured using the General Self-Efficacy Scale (21), the Moorong Self-Efficacy Scale (22), the General Belongingness Scale (23) and the MDS (17). In addition, the survey collected participants’ basic sociodemographic data and socioeconomic characteristics.
Statistical analysis
This study uses descriptive analysis of the evaluated data, presenting its results using absolute values, percentages, means and standard deviations. Excel 2013 for Windows (Microsoft Corporation, Redmond, Washington) was used to organize data and generate analyses.
RESULTS
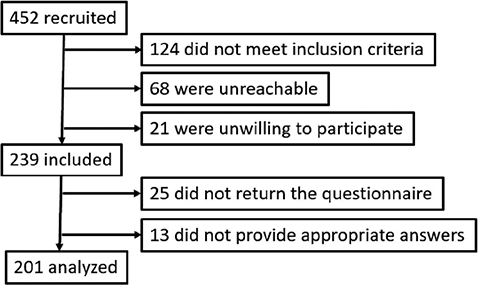
An initial total of 452 persons were recruited. Of these, 213 were were excluded, because they did not meet the inclusion criteria listed above (n = 124), they were not contactable (n = 68), or they declined to participate (n = 21). A total of 201 participants responded to the questionnaire and were included in the analyses. The remainder of study participants either (n = 38) did not return the questionnaire (n = 25) or did not provide appropriate answers (n = 13) and were therefore excluded from the analysis.
Of the 201 participants included in the analyses, 79% were male, they had an mean age 44 ± 17 years, age range 18–63 years, and 87% were living with other persons (all adults between 18 and 63 years old) (Figure 1).
Regarding education, 39% of participants completed secondary education only, followed by 24% who had a higher education degree largest subgroup. With reference to household income, 29% of the sample was within the range of 3 to 5 minimum wages. Minimum wage is the minimum wage a worker should receive from his employer.
Regarding the characteristics of the injury, 80% of the sample had an incomplete SCI and 60% had an injury at the thoracolumbar level (paraplegia). There was wide variation in the time since injury (3 ± 143 months) and in the causes of injury (Fig. 2). Traumatic aetiologies, such as interpersonal violence (including gunshot wounds) and road traffic accidents, were the main group of causes (19%), followed by degenerative spinal conditions (35%).
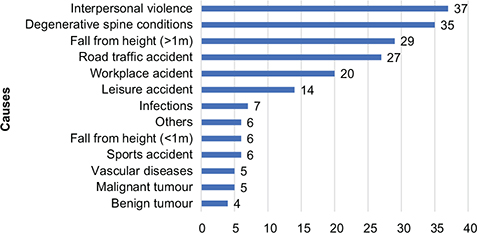
Fig. 2. Number of cause of injury (n = 201). The data is collected from International Spinal Cord Injury Survey.
Health conditions
Study participants considered spasticity their most problematic health condition (33%), followed by neuropathic pain (13%) (Table I). Participants’ perception of health was good in 47% of the study population, reasonable in 26%, very good in 15%, very bad in 6% and excellent in 6%.
Activity and participation
Data on activities and participation in society are related to individuals’ perception of social participation based on their personal choices and preferences. Approximately 50% of the study population reported not having any problem coping with activities of daily living and social roles, such as taking care of their health and interacting with others. However, 47% reported that it was very problematic to participate in many such activities (e.g. using public transport, helping others, and having sex).
Work
Seventy-seven percent of study participants reported being employed before injury onset. Only 16% of participants received vocational rehabilitation after the injury, while 84% did not receive any guidance or training to return to work. After rehabilitation, although 90% reported having never returnerd to work after the SCI and 20% were unemployed before the SCI.
Quality of life and general health
Forty-four percent of study participants reported having a good quality of life, while it was neither good nor poor for 33%, very good for 11%, very poor for 6%, and poor for 5%. Table II shows the results regarding participants’ satisfaction with several aspects of quality of life.
Environmental factors
The most relevant barriers that make the lives of people with SCI at least a little more difficult are the poor accessibility of public spaces and of means transportation for long distances, followed closely by the disabling barriers to accessing the homes of their friends and relatives and the lack of state services (Table III).
DISCUSSION
This study provides an evidence base regarding the lived experience of persons with SCI in south-eastern Brazil. By bringing together participants from 2 south-eastern states of Brazil, the study offers an overview of their living conditions, quality of life, and need for social support and healthcare services. A full understanding of the situation can only be obtained through participants’ reports of the issues that are significant to them. Currently, ongoing InSCI surveys are collecting data in 28 countries worldwide (4).
The results suggest that there is a need for interventions and public policies designed to improve overall accessibility and social participation. More specifically, many participants reported difficulty finding appropriate healthcare services that could address their health conditions.
In the current study is not a surprose (6, 7), Canada (9), Finland (24) and Switzerland (25) the large predominance of male participants (close to 80%) in the current study is not a surprise. This situation is quite similar for the distribution of participants across age groups, showing a relatively young adult population.
The study population is also comparable to that of other communities surveyed Australia in terms of severity levels of injuries, with quadriplegic persons accounting for approximately 40% of the SCI population, as per incidence levels generated from hospital records (26).
Previous studies have covered different aspects of the community life of persons with SCI by focusing on a combination of services (27, 28). Such studies have identified unmet needs for both healthcare and social participation, including work and employment, sexual activity and pain management, which are also reported in the current study.
In Canada, according to Hansen (29), accessible transportation and infrastructure are priority needs for people with SCI living in the community. Similarly, in the current study persons living with SCI in south-eastern Brazil identify physical barriers as major disabling environmental factors.
SCI-related health issues might impact quality of life (30) and increase chances to develop long-term secondary health conditions (31), increasing the need for appropriate healthcare services. As such, pain is a relevant condition reported in the current study, as in previous studies (32–34).
The current results suggest that persons with SCI report good performance in carrying out activities of daily living. However, they also report difficulties due to the lack of support and lack of accessible or assistive technologies. Hammel et al. (35) suggest that people with physical disability wish to define their own performance parameters instead of fulfilling various social norms.
Returning to work, for example, is often difficult. This study shows that only 10% of participants returned to work, reinforcing the results of a review that found low employment rates among persons with SCI (36).
On the other hand, quality of life is measured in terms of satisfaction with social participation and general health (37). The current study indicates good levels of satisfaction among subjects with SCI, regarding health, activities of daily living and with themselves, which might be related to the rehabilitation outcomes of the study population. Hill et al. (38) reported that high levels of quality of life are synonymous with positive results of rehabilitation treatment.
Study limitations
This study is the first of its kind in a Brazilian context to analyse several aspects of the lived experience of persons with SCI. The study has a number of limitations. First, the study population is restricted to participants from 2 well-resourced settings in south-eastern Brazil, which are not representative of the whole population. Secondly, some participants found it difficult to assess and express their perceptions of health, quality of life and disability, and to respond to survey questions. However, the study offers a wide evidence base on diverse topics. Finally, there are no questions specific to rehabilitation treatment of survey participants, which plays a decisive role in the health and participation in society of persons with SCI. However, this omission does not hinder the potential of the study to deliver on its objective.
CONCLUSION
This study was effective in creating a sound evidence base about the lived experience of persons with SCI in south-eastern Brazil. This is the first study to present detailed data regarding personal characteristics, associated health conditions, quality of life, work status, environmental factors, and other functioning-related aspects in this population. The data show that most of the survey respondents with SCI in south-eastern Brazil are male (79%) and paraplegic (60%), and they consider spasticity their most problematic health conditions (33%). Although the study subjects report having a good quality of life (44%), they still encounter disabling environmental barriers that make their life more difficult, such as poor accessibility of public spaces (61%) and means of transportation (58%), and only a small proportion (10%) return to work. This study provides an initial overview of the lived experience of people with SCI in south-eastern Brazil, based on self-reports of their health and socioeconomic conditions and functioning status. The results will serve as a starting point for future research on this population.
REFERENCES
- BRASIL. General health coordination of persons with disabilities. Brasília: Ministry of Health. Health Care Department. Department of Strategic Programmatic Actions; 2015.
- Singh A, Tetreault L, Kalsi-Ryan S, Nouri A, Fehlings MG. Global prevalence and incidence of traumatic spinal cord injury. Clin Epidemiol 2014; 6: 309–331. https://doi.org/10.2147/CLEP.S68889
- Gross-Hemmi MH, Post MWM, Ehrmann C, Fekete C, Hasnan N, Middleton JW, et al. Study protocol of the international spinal cord injury (InSCI) community survey. Am J Phys Med Rehabil 2017; 96: 23–34. https://doi.org/10.1097/PHM.0000000000000647
- Bickenbach JE, Officer A, Shakespears T, von Groote P. International perspectives on spinal cord injury. Geneva: WHO Press; 2013.
- Kurtzke JF, Epidemiology of spinal cord injury. Exp Neirol 1975; 48: 163–236. https://doi.org/10.1016/0014-4886(75)90175-2
- Botelho RV, Albuquerque LDG, Junior RB, Junior AAA. Epidemiology of traumatic spinal injuries in Brazil: systematic review. Arq Bras Neurocir 2014; 33: 100–106. https://doi.org/10.1055/s-0038-1626255
- Masini, M. Estimativa da incidência e prevalência de lesão medular no Brasil [An estimation of incidence and prevalence of spinal cord injury in Brazil]. J Bras Neurocirurg 2001; 12: 97–100. https://doi.org/10.22290/jbnc.v12i2.385
- Blanes L, Lourenço L, Carmagnani MIS, Ferreira LM. Clinical and sócio-demographic characteristics of person with traumatic paraplegia living in São Paulo, Brazil. Arq neuropsiquiatr 2009; 67: 388–390. https://doi.org/10.1590/S0004-282X2009000300003
- Brinkhof MWG, Fekete C, Chamberlain JD, Post MWM, Gemperli A, for the SwiSCI Study Group. Swiss national community survey on functioning after spinal cord injury: protocol, characteristics of participants and determinants of nonresponse. J Rehabil Med 2016; 48: 120–130. https://doi.org/10.2340/16501977-2050
- Fekete C, Segerer W, Gemperli A, Brinkhof MWG, for the SwiSCI Study Group. Participation rates, response bias and response behaviours in the community survey of the Swiss Spinal Cord Injury Cohort Study (SwiSCI). BMC Med Res Methodol 2015; 15: 80. https://doi.org/10.1186/s12874-015-0076-0
- World Health Organization (WHO). ICF – International Classification of Functioning, Disability and Health. Geneva: WHO Press; 2001.
- Cieza A, Kirchberger I, Biering-Sorensen F, Baumberger M, Charlifue S, Post MW, et al. ICF Core Sets for individuals with spinal cord injury in the long-term context. Spinal Cord 2010; 48: 305–312. https://doi.org/10.1038/sc.2009.183
- Kirchberger I, Cieza A, Biering-Sorensen F, Baumberger M, Charlifue S, Post MWM, et al. ICF Core Sets for individuals with spinal cord injury in the early post-acute context. Spinal Cord 2010; 48: 297–304. https://doi.org/10.1038/sc.2009.128
- Utiyama DMO, Alfieri FM, Battistella LR. Population survey on the functionality of people with spinal cord injury in Brazil: a protocol study. Acta Fisiatr 2020; 27: 11–19. https://doi.org/10.11606/issn.2317-0190.v27i1a172051
- Ware JE Jr, Sherbourne CD. The MOS 36-item Short-Form health survey (SF-36). I. Conceptual framework and item selection. Med Care 1992; 30: 473–483. https://doi.org/10.1097/00005650-199206000-00002
- Kalpakjian CZ, Scelza WM, Forchheimer MB, et al. Preliminary reliability and validity of a Spinal Cord Injury Secondary Conditions Scale. J Spinal Cord Med 2007; 30: 131–139. https://doi.org/10.1080/10790268.2007.11753924
- World Health Organization, The World Bank. Model Disability Survey (MDS). [accessed 2016 Mar 24]. Available from: http://www.who.int/disabilities/data/mds/en/
- Fekete C, Eriks-Hoogland I, Baumberger M, Catz A, Itzkovich M, Lüthi H, et al. Development and validation of a self-report version of the Spinal Cord Independence Measure (SCIM III). Spinal Cord 2013; 51: 40–47. https://doi.org/10.1038/sc.2012.87
- Jette AM, Slavin MD, Ni P, Kisala PA, Tulsky DS, Heinemann AW, et al. Development and initial evaluation of the SCI-FI/AT. J Spinal Cord Med 2015; 38: 409–418. https://doi.org/10.1179/2045772315Y.0000000003
- Ballert CS, Post MW, Brinkhof MW, Reinhardt JD; SwiSCI Study Group. Psychometric properties of the Nottwil Environmental Factors Inventory Short Form. Arch Phys Med Rehabil 2015; 96: 233–240. https://doi.org/10.1016/j.apmr.2014.09.004
- Schwarzer R, Jerusalem M: Generalized Self-Efficacy Scale. In, Weinman J, Wright S, Johnston M, editors. Measures in health psychology: a user’s portfolio. Causal and control beliefs. Windsor, UK: NFER-NELSON; 1995, p. 35–37. https://doi.org/10.1037/t00393-000
- Middleton J, Tate R, Geraghty T. Self-efficacy and spinal cord injury: psychometric properties of a new scale. Rehabil Psychol Health Med 2003; 48: 281–288. https://doi.org/10.1037/0090-5550.48.4.281
- Malone GP, Pillow D, Osman A. The General Belongingness Scale (GBS): assessing achieved belongingness. Personal Individ Differ 2012; 52: 311–316. https://doi.org/10.1016/j.paid.2011.10.027
- Noreau L, Noonan V, Cobb J, Leblond J, Dumont F. Spinal cord injury community survey: a national, comprehensive study to portray the lives of Canadians with spinal cord injury. Top Spinal Cord Inj Rehabil 2014; 20: 249–264. https://doi.org/10.1310/sci2004-249
- Tallqvist S, Antilla H, Kallinen M, Koskinen E, Hamalainen H, Kauppila A, et al. Health, functioning and accessibility among spinal cord injury population in Finland: protocol for the FinSCI study. J Rehabil Med 2019; 51: 273–280. https://doi.org/10.2340/16501977-2539
- New PW, Simmonds F, Stevermuer T. A population-based study comparing traumatic spinal cord injury and non-traumatic spinal cord injury using a national rehabilitation database. Spinal Cord 2011; 49: 397–403. https://doi.org/10.1038/sc.2010.77
- Kennedy P, Lude P, Taylor N. Quality of life, social participation, appraisals and coping post spinal cord injury: a review of four community samples. Spinal Cord 2006; 44: 95–105. https://doi.org/10.1038/sj.sc.3101787
- Cox RJ, Amsters DI, Pershouse KJ. The need for a multidisciplinary outreach service for people with spinal cord injury living in the community. Clin Rehabil 2001; 15: 600–606. https://doi.org/10.1191/0269215501cr453oa
- Rick Hansen Man-in-Motion Foundation (RHMIMF). SCI Forum report. Ipsos Reid 2005; 66: 7.
- Hammell KRW. Spinal cord injury rehabilitation research: patient priorities, current deficiencies and potential directions. Disabil Rehabil 2010; 32: 1209–1218. https://doi.org/10.3109/09638280903420325
- Hetz SP, Latimer AE, Arbour-Nicitopoulos KP, Martin Ginis KA. Secondary complications and subjective well-being in individuals with chronic spinal cord injury: associations with self-reported adiposity. Spinal Cord 2011; 49: 266–272. https://doi.org/10.1038/sc.2010.100
- Ataoglu E, Tiftik T, Kara M, Tunc H, Ersoz M, Akkus S. Effects of chronic pain on quality of life and depression in patients with spinal cord injury. Spinal Cord 2013; 51: 23–26. https://doi.org/10.1038/sc.2012.51
- Budh CN, Osteraker AL. Life satisfaction in individuals with a spinal cord injury and pain. Clin Rehabil 2007; 21: 89–96. https://doi.org/10.1177/0269215506070313
- Modirian E, Pirouzi P, Soroush M, Karbalaei-Esmaeili S, Shojaei H, Zamani H. Chronic pain after spinal cord injury: results of a long-term study. Pain Med 2010; 11: 1037–1043. https://doi.org/10.1111/j.1526-4637.2010.00865.x
- Hammel J, Magasi S, Heinemann A, Whiteneck G, Bogner J, Rodriguez E. What does participation mean? An insider perspective from people with disabilities. Disabil Rehabil 2008; 30: 1445–1460. https://doi.org/10.1080/09638280701625534
- Lidal IB, Hynh TK, Biering-Sorensen F. Return to work following spinal cord injury: a review. Disabil Rehabil 2007; 29: 1341–1375. https://doi.org/10.1080/09638280701320839
- Lund ML, Nordlund A, Bernspang B, Lexell J. Perceived participation and problems in participation are determinants of life satisfaction in people with spinal cord injury. Disabil Rehabil 2007; 29: 1417–1422. https://doi.org/10.1080/09638280601029068
- Hill MR, Noonan VK, Sakakibara BM, Miller WC; SCIRE Research Team. Quality of life instruments and definitions in individuals with spinal cord injury: a systematic review. Spinal Cord 2010; 48: 438–450. https://doi.org/10.1038/sc.2009.164
