ORIGINAL REPORT
MODELLING LONG-TERM OUTCOMES AND RISK OF DEATH FOR PATIENTS WITH POST-STROKE SPASTICITY RECEIVING ABOBOTULINUMTOXINA TREATMENT AND REHABILITATION THERAPY
Klemens FHEODOROFF, MD1, Natalya DANCHENKO, PhD2, John WHALEN, BSc, MBA2, Jovita BALCAITIENE, MD2, Bárbara MAGALHÃES, PhD3, Elzbieta SZULC, PhD3, Andrea ZAFFALON, PhD3, Mariya BURCHAKOVA, MD4, Dmitry NECHIPORENKO, MD4, Sean ROBBINS, MSc3
*John Whalen and Jovita Balcaitiene are former employees of Ipsen.
From 1Gailtal-Klinik, Hermagor, Austria, 2Ipsen, Boulogne-Billancourt, France, 3LatticePoint Consulting, Geneva, Switzerland and 4Ipsen, Moscow, Russia
Objective: Stroke is associated with a high risk of death and cardiovascular events. Rehabilitation therapy is critical for functional recovery, to reduce hospital readmissions, all-cause and cardiovascular mortality, and stroke recurrence (long-term outcomes). Post-stroke spasticity may prevent effective recovery by restricting mobility. AbobotulinumtoxinA is an adjunctive therapy to physical therapy for post-stroke spasticity, but its long-term effects are unknown. The objective was to model the long-term clinical and economic outcomes of abobotulinumtoxinA for post-stroke spasticity.
Methods: Effects of abobotulinumtoxinA on treating post-stroke spasticity and evidence linking functional outcomes with long-term outcomes were collected in a focused literature review. A model was developed to estimate health benefits on long-term outcomes, direct medical costs, life- and quality-adjusted life-years for abobotulinumtoxinA injections plus rehabilitation therapy compared with rehabilitation therapy alone, from a UK perspective over a 10-year time-period.
Results: AbobotulinumtoxinA + rehabilitation therapy led to a risk reduction of 8.8% for all-cause mortality, and an increase of 13% in life-years and 59% in quality-adjusted life-years compared with rehabilitation therapy alone. AbobotulinumtoxinA + rehabilitation therapy was considered cost-effective compared with rehabilitation therapy alone (incremental cost-effectiveness ratio: £24,602).
Conclusion: AbobotulinumtoxinA + rehabilitation therapy may improve long-term outcomes, including post-stroke survival, while being cost-effective for the treatment of post-stroke spasticity.
LAY ABSTRACT
Here we developed a model to explore and compare the long-term benefits and overall costs of two interventions for the treatment of post-stroke spasticity (PSS): abobotulinumtoxinA injections plus rehabilitation therapy (aboBoNT-A+RT) vs. RT alone. Stroke survivors are known to be at a higher risk of recurrent stroke and death, and more than 25% are affected by spasticity. PSS significantly reduces patients’ mobility, physical functioning, and subsequently their ability to recover after a stroke. AboBoNT-A+RT is an effective treatment for spasticity. This model is the first to highlight that combining aboBoNT-A injections with RT could improve the overall survival of stroke survivors with spasticity by 8.8% and their overall quality of life, while being considered good value for money by UK payers.
Key words: stroke; spasticity; abobotulinumtoxinA; rehabilitation; cost-effectiveness analysis; mortality; United Kingdom.
Citation: J Rehabil Med 2022; 54: jrm00303. DOI: https://dx.doi.org/10.2340/jrm.v54.2422
Copyright: © Published by Medical Journals Sweden, on behalf of the Foundation for Rehabilitation Information. This is an Open Access article distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (https://creativecommons.org/licenses/by-nc/4.0/)
Accepted: Jun 16, 2022; Epub ahead of print: Jul 18, 2022; Published: Aug 24, 2022
Correspondence address: Natalya Danchenko, 13, rue de l’Avre, Paris 75015. Email: natalyadanchenko7@gmail.com
Stroke is the second most common cause of death and disability in Europe; it affects more than 1 million inhabitants of Europe every year (1). In 2017, there were 9.53 million stroke survivors in Europe. A significant proportion of stroke survivors will experience recurrent stroke, with 5-year cumulative incidence rates ranging from 16% to 30% (2, 3). First-ever ischaemic stroke is also associated with an increased risk of major adverse cardiovascular (CV) events in the first year after a stroke (4–6). Projections show that with no effective prevention strategy, including secondary prevention, the burden of stroke will not decrease in the next decade and beyond (7). To reduce the risks of death, secondary stroke and secondary major CV events (i.e. acute coronary syndrome, myocardial infarction, incident coronary artery disease, incident heart failure or CV death), and to foster physical recovery, stroke rehabilitation guidelines recommend that patients should engage in aerobic physical activity sessions to tackle physical inactivity (8, 9).
Stroke survivors may encounter distinct barriers to physical activity. Notably, 25.3% of survivors develop post-stroke spasticity (PSS) over the first year after a stroke, and they may also experience motor weakness, altered perception and balance, and impaired cognition that would result in inability to participate in exercise programmes (8, 10, 11).
Spasticity describes involuntary muscle hyperactivity in the presence of central paresis (12). Spasticity is generally associated with 1 or more lesions involving both the pyramidal and extrapyramidal tracts (13). As a result, spasticity can be a source of pain, discomfort and deformities, and can be a major barrier to physical exercise (8).
Treatment of spasticity often involves a combination of physical and pharmacological interventions, which can improve physical function and reduce secondary complications. AbobotulinumtoxinA therapy (aboBoNT-A; Dysport®, Ipsen Pharma, Boulogne-Billancourt, France) is a well tolerated and effective treatment for PSS of the upper and lower limbs (14, 15) that improves rehabilitation outcomes (16, 17) and relieves pain (18). AboBoNT-A treatment is also effective in improving patients’ quality of life (19).
Patients generally experience rapid improvement with aboBoNT-A therapy, thus clinical trials are of short duration. Consequently, it is not known if treatment-related improvements in mobility could also contribute to lowering the risks of CV events and all-cause death.
To assess if aboBoNT-A injections could also have an impact on long-term outcomes, a 10-year survival model was developed that compares the effects of aboBoNT-A injections and rehabilitation therapy (aboBoNT-A + RT) with rehabilitation therapy (RT) alone.
METHODS
Survival model structure
An exploratory 3-state model was developed using Microsoft Excel (Microsoft Office 365, Redmond, WA, USA) to estimate long-term outcomes (all-cause mortality and subsequent CV events), direct medical costs, life-years and quality-adjusted life-years (QALYs) of 2 interventions in PSS: aboBoNT-A + RT and RT alone, with RT encompassing all interventions aimed at improving the physical functioning and mobility of post-stroke survivors with spasticity (e.g. general physiotherapy aimed at improving movement and balance, cardiorespiratory and resistance training, strength exercise, etc.). The modelling was performed from a UK payer perspective over a 10-year time-period. The incremental costs per QALYs gained, ICER (incremental cost-effectiveness ratio), of aboBoNT-A + RT vs RT alone was calculated.
No studies of aboBoNT-A have evaluated the impact of aboBoNT-A injections on all-cause death and CV event risks. Thus, a focused literature review (FLR) was performed to search for evidence, with 2 objectives. First, to quantify the effect of botulinum toxin A (BoNT-A) on measures of disability for patients with PSS. Secondly, to quantify the association between measures of disability and long-term outcomes, such as death and secondary CV events, in stroke survivors (see Supplementary methods).
Publications identified in the FLR are available in the Supplementary materials (Tables SV and SVI). Of the evidence identified in the FLR, the Functional Independence Measure (FIM) was the only functional outcome that allowed us to model the effect of aboBoNT-A injections on all-cause mortality. There was insufficient evidence to compute a link between other disability or functional outcomes and long-term outcomes. The effect of aboBoNT-A injections on FIM score was studied in a randomized controlled study, and the gain in FIM score after rehabilitation was associated with a reduction in the risk of all-cause mortality in stroke survivors (20–22). When applicable, summary effect(s) for functional and long-term outcomes were computed with meta-analyses, using the random effect model in R (R core Team, 2021) [The R Foundation for Statistical Computing, Vienna, Austria] and the metafor package (23) (Table SII).
All patients in the model were followed for adverse events, time in PSS, and long-term outcome health states and death. In both interventions, patients were assumed to continue treatment for the duration of the 10-year time-period. The time in each health state was derived from survival data for stroke survivors.
Survival data
Four publications were considered as sources of data for overall survival after the first stroke (24–27). Because it is well known that a significant proportion of stroke survivors develop spasticity symptoms after the first stroke, these studies were considered to be relevant for our modelled patient population. To build the model, it was assumed that base overall survival rates of stroke survivors were identical for patients with or without spasticity symptoms. Kaplan–Meier survival curves from all studies were digitalized with WebPlotDigitizer (28) and reconstructed with Weibull or Gompertz parametric models (Figs S1–S4). The best model was selected based on the Akaike and Bayesian information criteria, and visual inspection, according to best practice in extrapolation of survival data (29). In the base-case analysis, the extrapolated survival data of post-stroke patients reported by Wolfe and colleagues was used (24).
Intervention-specific survival probabilities were computed based on modelled hazard ratios (HRs) derived from the evidence identified in the FLR, assuming that the proportional hazard condition would be met (calculations are detailed in the Supplementary methods). Probabilities of non-fatal recurrent stroke and CV events were derived from the literature (3, 30).
Utility, resource identification, quantification and valuation
In the base case, healthcare resource utilization data were based on a cost-utility analysis of aboBoNT-A for PSS (31) (Table I). This study was selected as the best source of data for our model, because it included healthcare resource utilization and quality of life (as utility value) data for patients with either lower- or upper-limb spasticity or both, while other studies focused on upper-limb spasticity (32–36). Hourly rates of community-based and hospital-based healthcare services were derived from Unit Costs of Health & Social Care 2020, funded by the National Institute for Health Research UK (37). Unit costs of inpatient and outpatient healthcare services were collected from the National Health Service (NHS) UK Cost Collection 2018/2019 (Table II). The aboBoNT-A injection schedule was derived from the UK label (Dysport®, Ipsen, retrieved from medicines.org.uk in July 2021). All costs and health benefits were discounted by 3.5%, according to the National Institute for Health and Care Excellence (NICE) guide to the methods of technology appraisal (9). In the model, patients in the aboBoNT-A + RT intervention were assumed to receive an injection every 12 weeks and to continue treatment for the entirety of the modelled time-period. Twelve weeks is the minimal interval between aboBoNT-A injections based on the Dypsort® label (UK, April 2021), making it a conservative assumption for our model.
| Parameter | Estimate | Reference – assumption |
| Toxin acquisition and administration | ||
| Cost of a toxin vial, £ | 154 | Dysport®, UK, Ex-MAN (50) |
| Toxin dose in the vial, U | 500 | |
| Administration cost – outpatient setting, £/h | 47.33 | Community-based physiotherapist (mean cost of a specialist from bands 5, 6, 7) – calculated from Curtis et al., 2020 (37) |
| Administration cost – day hospital, £ per h | 49.67 | Hospital-based physiotherapist (mean cost of a specialist from bands 5, 6, 7) – calculated from Curtis et al., 2020 (37) |
| Healthcare services | ||
| Follow-up visits, £/unit | 58.00 | One-time cost of outpatient physiotherapy – NHS costs 2018–19 (51) |
| Rehabilitation in day hospital, £/h | 49.67 | Hospital-based physiotherapist (mean cost of a specialist from bands 5, 6, 7) – calculated from Curtis et al., 2020 (37) |
| Rehabilitation in outpatient or home setting, £/h | 47.33 | Community-based physiotherapist (mean cost of a specialist from bands 5, 6, 7) – calculated from Curtis et al., 2020 (37) |
| Home care, £/h | 27.29 | Weighted mean cost of home care per h (£24 per weekday h, £30 per face-to-face per weekday h, £25 per day-time weekend, £30 per face-to-face per day-time weekend) – calculated from Curtis et al., 2020 (37) |
| Intrathecal pump set-up, £ | 8 764.00 | One-time cost of insertion of intrathecal drug delivery device for treatment of neurological conditions, 19 years and over – calculated based on NHS costs 2018–19 (51) |
| Baclofen cost, £/mg | 0.28 | Mean price available in the UK (50) |
| Baclofen intrathecal cost, £/mg | 5.42 | Mean price available in the UK (50) |
| Gabapentin cost, £/mg | 0.06 | Mean price available in the UK (50) |
| Cost of a secondary stroke event, £ | 4 750.71 | Mean cost per hospitalization, stroke, NHS costs 2018–19 (51) |
| Cost of a CV event, £ | 2 366.94 | Mean cost per hospitalization, actual or suspected myocardial infarction, NHS costs 2018–19 (51) |
| Adverse events – botulism, £/unit | ||
| Electromyographies | 199.00 | Assumed to be identical to one time cost of conventional EEG, EMG or nerve conduction studies, 19 years and over in the hospital setting – NHS costs 2018–19 (51) |
| Physiatrist visit in outpatient setting | 58.00 | One-time cost of outpatient physiotherapy – NHS costs 2018–19 (51) |
| Neurologist visits in outpatient setting | 177.00 | One-time cost of neurologist attendance – NHS costs 2018–19 (51) |
| Rehabilitation sessions in outpatient setting | 58.00 | One-time cost of outpatient physiotherapy – NHS costs 2018–19 (51) |
| CV: cardiovascular; EEG: electroencephalography; EMG: electromyography; NHS: National Health Service. | ||
Sensitivity analyses
A 1-way deterministic sensitivity analysis (DSA) was conducted by altering data inputs for key model variables. A probabilistic sensitivity analysis (PSA) was also conducted, with distributions assigned to key model variables and utility scores, by random sampling (1000 iterations). Uncertainties associated with utility scores were described by the β distribution, while uncertainties associated with costs and healthcare resource utilization were described by the γ distribution. Standard error for parameters were retrieved from the Lazzaro study (31) or they were assigned an appropriate (10%) coefficient of variation on their point estimate (38) (Table SVIII).
A second deterministic sensitivity analysis was performed to assess the impact of resource utilization estimates on incremental costs and the ICER. In this analysis, resource utilization data reported by Ward and colleagues (based on the UK healthcare practice) were used instead of the estimates reported by Lazzaro and colleagues, the latter being more conservative from a cost perspective (31, 33). It was assumed that estimates reported by Ward and colleagues (Table SX), although restricted to upper-limb spasticity, could reflect the benefit of aboBoNT-A injections for the treatment of both upper- and lower-limb spasticity on resource utilization in UK clinical practice.
RESULTS
A review of the literature identified FIM score as an efficacy outcome that could be used to model the effect of aboBoNT-A injections on all-cause mortality in post-stroke patients treated for spasticity. Stroke survivors who reported greater improvement in FIM score during rehabilitation had lower risk of all-cause mortality during follow-up (summary effect HR per 1-point gain in FIM: 0.9626, 95% confidence interval (95% CI) 0.9245–1.0022) (21, 22). Patients treated with aboBoNT-A injections + RT showed greater improvement in FIM score than patients treated without aboBoNT-A injections (Table SII) (20).
The modelling results showed that the addition of aboBoNT-A injections to RT led to a reduction of 8.8% in the risk of all-cause mortality, and a relative increase of 12.8% in discounted life-years (Table III). The addition of aboBoNT-A injections to RT led to an increase of £42,328 in total costs over 10 years, including £9,520 for drug acquisition and £743 for drug administration. In the base-case scenario, incremental costs were driven by the increased number of hours of home care and RT for patients treated with aboBoNT-A injections compared with RT alone, as reported by Lazzaro and colleagues (31).
Although a small change in life-years in favour of aboBoNT-A + RT was observed, the change in QALYs was more substantial. Over the 10-year period, aboBoNT-A + RT led to more QALYs than RT alone (4.647 vs 2.926, respectively) (Table III).
Overall, the ICER of aboBoNT-A injections was £24,602 per QALY, which is below the current upper threshold of £30,000 to be considered a cost-effective use of resources in the UK.
All of the evaluated scenario analyses remained under £30,000 per QALY gained. One scenario (using resource utilization data published by Ward and colleagues) found aboBoNT-A + RT to be cost saving compared with RT alone (£168,274 vs £171,330, respectively); in this scenario, aboBoNT-A + RT was economically dominant (Table SXI) (33).
According to UK national guidelines, patients usually should be reinjected when spasticity symptoms start to reoccur (39). In a previous longitudinal study of upper-limb spasticity, the mean time interval between aboBoNT-A injections was 156.4 days (22.3 weeks) (40). In the model, 3 different aboBoNT-A regimens were tested, with aboBoNT-A injections every 12 weeks (3 months), 16 weeks (4 months) and 24 weeks (6 months). The price of an aboBoNT-A vial remained unchanged. The ICER associated with each different dosing timing (12, 16 and 24 weeks) was £24,602, £23,110 and £21,618, respectively.
In the base-case scenario, we selected the study by Wolfe and colleagues, a registry study performed in the UK, to extrapolate the survival probabilities of stroke survivors with spasticity, while we also identified additional sources of data in the literature (24–27). Changing the source of overall survival data led to an increase in the ICER (range: £24,405–28,877) (Table SVII and Table SIX).
A DSA was conducted to determine the model parameters contributing the greatest uncertainty to the model results. The DSA of the base-case analysis showed that home care (i.e. number of hours and costs), base HR for all-cause mortality, effect of aboBoNT-A + RT (or RT alone) on the functional outcome, quality of life and the cost of an aboBoNT-A vial were the parameters with the greatest influence on the ICER (Table IV). In general, the ICER remained under the £30,000 threshold, except in the low value for aboBoNT-A + RT subsequent year(s) utility value (−1 SD from the point estimate) and the high value for the HR for all-cause mortality (upper bound of the 95% CI).
Joint parameter uncertainty was explored with a PSA. In the base-case analysis, the SD of healthcare resource use parameters (i.e. number of follow-up visits per year, hours of rehabilitation in day hospital per year, hours of RT in outpatient or home setting per year, and the number of hours of home care per year) was set to 10% of the deterministic mean reported by Lazzaro and colleagues (31). A cost-effectiveness acceptability curve was generated to illustrate the probability that each strategy is cost-effective at varying levels of willingness to pay (Fig. 1). The PSA demonstrated a 73% likelihood that aboBoNT-A + RT is cost-effective compared with RT alone at an ICER threshold of £30,000. The results of the PSA are also represented in the cost-effectiveness plane scatterplot in Fig. 2, which demonstrates the results of 1,000 simulations.
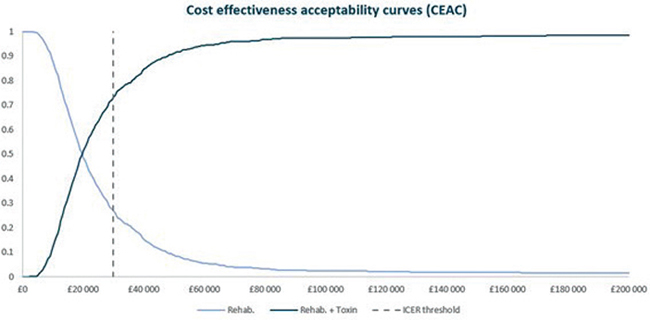
Fig. 1. Cost-effectiveness acceptability curve for the base-case scenario analysis. aboBoNT-A + RT: abobotulinumtoxinA injections plus rehabilitation therapy; RT: rehabilitation therapy alone.
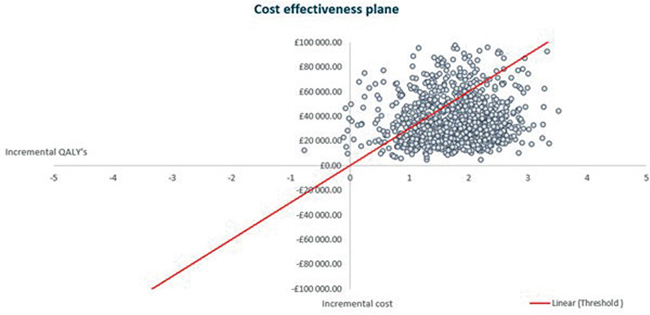
Fig. 2. Cost-effectiveness plane; aboBoNT-A + RT compared with RT alone. AboBoNT-A + RT: abobotulinumtoxinA injections plus rehabilitation therapy; RT: rehabilitation therapy.
A second PSA analysis was performed to explore the uncertainty related to the variance of the model inputs. In this analysis, the SD parameter of the sampling distribution for the healthcare resource use parameters was considered to be equal to the deterministic mean. This analysis showed that the likelihood of aboBoNT-A + RT being considered to be cost-effective against RT alone at an ICER threshold of £30,000 was 68% (Figs S5 and S6).
DISCUSSION
This analysis found that aboBoNT-A + RT compared with RT alone could reduce the risk of all-cause mortality by 8.8%, which can be considered to be highly important by decision-makers and relevant to patients. This is the first study to quantify the possible survival gain associated with physical function improvement for people with PSS. In the elderly population, physical activity is associated with improved overall health (41), including lower risk of CV events (42). Benefits resulting from physical activity in healthy individuals are also relevant to stroke survivors (43), who experience increased risks of recurrent stroke (2, 3, 30) and major adverse CV events (4–6). Immobility, motor weakness, and altered perception and balance experienced by stroke survivors greatly hinder their ability to follow clinical recommendations to tackle physical inactivity (8). Spastic symptoms, which occur in a significant proportion of stroke survivors, further contribute to the barriers to physical exercise (19).
Here, we modelled the effect of aboBoNT-A injections on all-cause mortality using a functional or a disability outcome as a linking variable. Given the lack of long-term studies of aboBoNT-A injections for PSS, treatment effects were modelled based on 1 randomized clinical trial assessing the benefit of aboBoNT-A injections on FIM score in patients with PSS, and 2 studies reporting a statistically significant association between gain in FIM score after post-stroke rehabilitation and the risk of all-cause mortality (20–22).
The literature search identified only 1 study reporting healthcare resource utilization data in stroke survivors with either upper- or lower-limb spasticity (31). This cost-utility analysis was performed from the Italian National Health Service perspective, and found that combining aboBoNT-A injections with RT resulted in a higher number of QALYs gained than with RT alone (1.620 vs 1.150, respectively), and incremental cost-utility ratios of €12,341 and €23,600 for the Italian NHS and societal perspectives, respectively. These results are consistent with our finding of 1.71 QALYs gained and an ICER of £24,602 per QALY gained. Other pharmaco-economic studies have assessed the benefit of BoNT-A injections compared with best supportive care in adult upper-limb spasticity (31–36), but these also had short time-periods and did not attempt to quantify treatment effects on mortality or secondary CV events. However, most of these studies concluded that BoNT-A injections are a cost-effective treatment for PSS (31, 33, 34, 36).
Extensive sensitivity analyses consistently found aboBoNT-A injections to be cost-effective. In the probabilistic analysis, 73% of simulations found an ICER below £30,000. A scenario considering alternative sources of resource utilization data (32, 33) found lower utilization of day hospital, day centre or physiotherapist resources, such that aboBoNT-A was cost saving and associated with a negative ICER. In addition, our base-case scenario assumed that patients were treated with aboBoNT-A for 10 years, with injection intervals of 12 weeks, according to the Dysport® label. In UK clinical practice, patients may undergo aboBoNT-A therapy for shorter periods of time and with longer time intervals between injections (40), leading to a lower incremental cost in the current analysis. Consequently, costs associated with aboBoNT-A therapy are conservative and likely to be overestimated in the current model.
Although BoNT-A therapy has been shown to be cost-effective for the treatment of post-stroke patients with upper-limb spasticity (31–34), the results of the current study show that it could also have a benefit for all-cause mortality, while remaining cost-effective. However, this study has several limitations. First, extensive healthcare resource utilization and quality of life data representative of the UK clinical practice for post-stroke patients with spasticity, independently of the limb affected (upper or lower limb), were not available in the literature. Consequently, the current study relied on data from Lazzaro and colleagues (31), which were based on the Italian clinical setting. Secondly, this model used evidence produced in a single randomized clinical trial assessing the effect of aboBoNT-A injections on FIM score after rehabilitation (20). However, another study (non-randomized, thus not included in the model) found that BoNT-A injections had a positive effect on FIM score (44).
AboBoNT-A therapy improves rehabilitation outcomes on functional independence (16, 17, 19) in patients with PSS, and several studies have shown that BoNT-A injections can decrease the burden of care of long-term care residents treated for upper- and lower-limb spasticity (45–47). The current model assessed the impact of aboBoNT-A injections on all-cause mortality, using FIM score as a linking variable. BoNT-A injections are known to improve disability, physical functioning and mobility, and the Barthel Index or the 6-minute walk test are often used to assess and report these improvements (Table SV). Some of the outcomes used in BoNT-A studies are associated with long-term outcomes in stroke survivors or in elderly patients (Tables SIII and SIV). However, the way the evidence was reported in the literature did not enable us to use different outcomes from FIM score as linking variables to model the effect of aboBoNT-A injections on all-cause mortality or CV events.
CONCLUSION
This is the first model to suggest that aboBoNT-A therapy may have additional long-term benefits that are not captured in spasticity-focused trials. AboBoNT-A injections significantly improve limb spasticity and mobility, enabling patients to regain some level of functional independence, while also reducing pain and caregiver burden (18, 20, 45–47). Improving patient mobility is also important to lower the risk of deep vein thrombosis and pressure ulcers, which can lead to infections (48, 49). It is clear that enabling funding for repeated aboBoNT-A injections is important, and this is supported by the evidence of a large international study that demonstrated the benefit of repeated cycles of aboBoNT-A, over 2 years captured through personcentred goal attainment and standardized measures (40).
The long-term survival rates of stroke survivors with spasticity have not been captured and reported in the literature. Therefore, the model was built based on survival rates of stroke survivors, knowing that a substantial proportion of these patients will have spasticity. While we assumed that these rates would be comparable to those of patients with spasticity, we anticipate that patients with spasticity and mobility impairments will have a lower life expectancy. Since the current model is comparing 2 intervention schemes in the same patient population, we do not expect this limitation to significantly alter the conclusion of this exploratory model. On the contrary, we consider that the model may underestimate the putative benefits of aboBoNT-A on the survival rates of stroke survivors with spasticity.
This study advocates for the need to consider and capture the impact of aboBoNT-A injections on all-cause mortality and secondary events, such as CV events and recurrent stroke, which are prevalent in stroke survivors (4–6). The model did not explore other long-term outcomes, such as pain or the burden of caregivers, which are also relevant to patients, caregivers and payers. Moreover, the current study did not explore the impact of treatment adherence or treatment discontinuation on the long-term benefits of aboBoNT-A injections.
In conclusion, the evidence reported in the literature and the results of this exploratory analysis strongly support the observation that aboBoNT-A injections are an effective use of resources for the treatment of PSS, with the potential to improve long-term outcomes, such as post-stroke survival. Future research will be beneficial to further test and validate the results and hypotheses presented in this study.
ACKNOWLEDGEMENTS
Competing interests
The authors have no conflicts of interest to declare.
Funding
This study was funded by Ipsen.
REFERENCES
- Wafa HA, Wolfe CDA, Emmett E, Roth GA, Johnson CO, Wang Y. Burden of stroke in Europe: thirty-year projections of incidence, prevalence, deaths, and disability-adjusted life years. Stroke 2020; 51 (8): 2418–2427.
- Elnady HM, Mohammed GF, Elhewag HK, Mohamed MK, Borai A. Risk factors for early and late recurrent ischemic strokes. Egypt J Neurol Psychiatry Neurosurg 2020; 56 (1): 0–6.
- Lin B, Zhang Z, Mei Y, Wang C, Xu H, Liu L, et al. Cumulative risk of stroke recurrence over the last 10 years: a systematic review and meta-analysis. Neurol Sci 2021; 42 (1): 61–71.
- Gunnoo T, Hasan N, Khan MS, Slark J, Bentley P, Sharma P. Quantifying the risk of heart disease following acute ischaemic stroke: a meta-analysis of over 50 000 participants. BMJ Open 2016; 6 (1): 1–7.
- Shima S, Shinoda M, Takahashi O, Unaki A, Kimura T, Okada Y, et al. Risk factors for acute heart failure and impact on in-hospital mortality after stroke. J Stroke Cerebrovasc Dis 2019; 28 (6): 1629–1635.
- Sposato LA, Lam M, Allen B, Shariff SZ, Saposnik G. First-ever ischemic stroke and incident major adverse cardiovascular events in 93 627 older women and men. Stroke 2020 Feb; 51(2): 387–394.
- Norrving B, Barrick J, Davalos A, Dichgans M, Cordonnier C, Guekht A, et al. Action plan for stroke in Europe 2018–2030. Eur Stroke J 2018; 3 (4): 309–336.
- Kernan WN, Ovbiagele B, Black HR, Bravata DM, Chimowitz MI, Ezekowitz MD, et al. Guidelines for the prevention of stroke in patients with stroke and transient ischemic attack: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 2014; 45: 2160–2236.
- NICE Guidance CG162 2013. Guide to the Methods of Technology Appraisal. Available from: https://www.nice.org.uk/process/pmg9/chapter/foreword. (Accessed: Thursday 11 March 2021)
- Zeng H, Chen J, Guo Y, Tan S. Prevalence and risk factors for spasticity after stroke: a systematic review and meta-analysis. Front Neurol. 2021 Jan 20;11:616097. Available from: https://www.frontiersin.org/articles/10.3389/fneur.2020.616097/full
- Winstein CJ, Stein J, Arena R, Bates B, Cherney LR, Cramer SC, et al. Guidelines for adult stroke rehabilitation and recovery: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 2016; 47 (6): e98–169. Available from: http://www.ncbi.nlm.nih.gov/pubmed/27145936
- Dressler D, Bhidayasiri R, Bohlega S, Chana P, Chien HF, Chung TM, et al. Defining spasticity: a new approach considering current movement disorders terminology and botulinum toxin therapy. J Neurol 2018; 265 (4): 856–862. Available from: https://doi.org/10.1007/s00415-018-8759-1
- Pandyan AD, Gregoric M, Barnes MP, Wood D, Van Wijck F, Burridge J, et al. Spasticity: clinical perceptions, neurological realities and meaningful measurement. Disabil Rehabil 2005; 27 (1–2): 2–6. Available from: http://www.ncbi.nlm.nih.gov/pubmed/15799140
- Gracies J-M, Brashear A, Jech R, McAllister P, Banach M, Valkovic P, et al. Safety and efficacy of abobotulinumtoxinA for hemiparesis in adults with upper limb spasticity after stroke or traumatic brain injury: a double-blind randomised controlled trial. Lancet Neurol 2015; 14 (10): 992–1001. Available from: http://dx.doi.org/10.1016/S1474-4422(15)00216-1
- Gracies J-M, Esquenazi A, Brashear A, Banach M, Kocer S, Jech R, et al. Efficacy and safety of abobotulinumtoxinA in spastic lower limb: randomized trial and extension. Neurology 2017; 89 (22): 2245–2253. Available from: http://www.ncbi.nlm.nih.gov/pubmed/29093068
- Demetrios M, Gorelik A, Louie J, Brand C, Baguley IJ, Khan F. Outcomes of ambulatory rehabilitation programmes following botulinum toxin for spas ticity in adults with stroke. J Rehabil Med 2014; 46 (8): 730–737.
- Gracies JM, O’Dell M, Vecchio M, Hedera P, Kocer S, Rudzinska-Bar M, et al. Effects of repeated abobotulinumtoxinA injections in upper limb spasticity. Muscle Nerve 2018; 57 (2): 245–254.
- Turner-Stokes L, Fheodoroff K, Jacinto J, Maisonobe P. Results from the Upper Limb International Spasticity Study-II (ULIS-II): a large, international, prospective cohort study investigating practice and goal attainment following treatment with botulinum toxin a in real-life clinical management. BMJ Open. 2013 Jun 20; 3(6): e002771. Available from: https://pubmed.ncbi.nlm.nih.gov/23794582/
- Rosales RL, Chua-Yap AS. Evidence-based systematic review on the efficacy and safety of botulinum toxin-A therapy in post-stroke spasticity. J Neural Transm 2008; 115 (4): 617–623.
- Pennati G V, Da Re C, Messineo I, Bonaiuti D. How could robotic training and botolinum toxin be combined in chronic post stroke upper limb spasticity? A pilot study. Eur J Phys Rehabil Med 2015; 51 (4): 381–387. Available from: http://www.ncbi.nlm.nih.gov/pubmed/25358636
- Maruyama K, Nakagawa N, Koyama S, Maruyama J-I, Hasebe N. Malnutrition increases the incidence of death, cardiovascular events, and infections in patients with stroke after rehabilitation. J Stroke Cerebrovasc Dis 2018; 27 (3): 716–723. Available from: https://doi.org/10.1016/j.jstrokecerebrovasdis.2017.10.002
- Scrutinio D, Monitillo V, Guida P, Nardulli R, Multari V, Monitillo F, et al. Functional gain after inpatient stroke rehabilitation: correlates and impact on long-term survival. Stroke 2015;46 (10): 2976–2980. Available from: http://www.ncbi.nlm.nih.gov/pubmed/26337968
- Viechtbauer W. Conducting meta-analyses in R with the metafor. J Stat Softw 2010; 36 (3): 1–48.
- Wolfe CDA, Crichton SL, Heuschmann PU, McKevitt CJ, Toschke AM, Grieve AP, et al. Estimates of outcomes up to ten years after stroke: analysis from the prospective South London Stroke Register. PLoS Med 2011; 8 (5): e1001033. Available from: http://www.ncbi.nlm.nih.gov/pubmed/21610863
- Cabral NL, Nagel V, Conforto AB, Amaral CH, Venancio VG, Safanelli J, et al. Five-year survival, disability, and recurrence after first-ever stroke in a middle-income country: a population-based study in Joinvile, Brazil. Int J Stroke 2018; 13 (7): 725–733. Available from: http://www.ncbi.nlm.nih.gov/pubmed/29513098
- Caro JJ, Ishak KJ, Migliaccio-Walle K. Estimating survival for cost-effectiveness analyses: a case study in atherothrombosis. Value Heal 2004; 7 (5): 627–635. Available from: http://dx.doi.org/10.1111/j.1524-4733.2004.75013.x
- Wang Y, Rudd AG, Wolfe CDA. Trends and survival between ethnic groups after stroke: the South London Stroke Register. Stroke 2013; 44 (2): 380–387.
- Rohatgi, A, WebPlotDigitizer 2020. Available from: https://automeris.io/WebPlotDigitizer
- NICE DSU Technical Support Document 14. Available from: https://nicedsu.sites.sheffield.ac.uk/tsds/completed-or-in-progress
- Dhamoon MS, Sciacca RR, Rundek T, Sacco RL, Elkind MSV. Recurrent stroke and cardiac risks after first ischemic stroke: The Northern Manhattan Study. Neurology 2006; 66 (5): 641–646.
- Lazzaro C, Baricich A, Picelli A, Caglioni PM, Ratti M, Santamato A. AbobotulinumtoxinA and rehabilitation vs rehabilitation alone in post-stroke spasticity: a cost-utility analysis. J Rehabil Med 2020; 52 (2). Available from: http://www.ncbi.nlm.nih.gov/pubmed/31820010
- Shaw L, Rodgers H, Price C, van Wijck F, Shackley P, Steen N, et al. BoTULS: A multicentre randomized controlled trial to evaluate the clinical effectiveness and cost-effectiveness of treating upper limb spasticity due to stroke with botulinum toxin type A. Health Technol Assess. 2010 May; 14(26): 1–113, iii–iv.
- Ward A, Roberts G, Warner J, Gillard S. Cost-effectiveness of botulinum toxin type a in the treatment of post-stroke spasticity. J Rehabil Med 2005; 37 (4): 252–257. Available from: http://www.ncbi.nlm.nih.gov/pubmed/16024483
- Makino K, Tilden D, Guarnieri C, Mudge M, Baguley IJ. Cost effectiveness of long-term incobotulinumtoxin-A treatment in the management of post-stroke spasticity of the upper limb from the Australian Payer Perspective. PharmacoEconomics – Open 2019; 3 (1): 93–102. Available from: https://doi.org/10.1007/s41669-018-0086-z
- Neusser S, Kreuzenbeck C, Pahmeier K, Lux B, Wilke A, Wasem J, et al. Budget impact of botulinum toxin treatment for spasticity after stroke – a German perspective. J Public Health 2019; 29:735–741.
- Rychlik R, Kreimendahl F, Schnur N, Lambert-Baumann J, Dressler D. Quality of life and costs of spasticity treatment in German stroke patients. Health Econ Rev 2016; 6 (1). Available from: http://dx.doi.org/10.1186/s13561-016-0107-5
- Curtis L. Unit Costs of Health & Social Care 2014. University of Kent, editor. PSSRU: Personal Social Services Research Unit. University of Kent; 2014. 1–292 p. Available from: http://www.pssru.ac.uk/project-pages/unit-costs/2014/index.php
- Briggs A, Claxton K, Sculpher M. Decision modelling for health economic evaluation. Oxford: Oxford University Press Inc.; 2006.
- The Royal College of Physicians. Spasticity in adults: management using botulinum toxin. National guidelines 2018. Available from: https://www.rcplondon.ac.uk/guidelines-policy/spasticity-adults-management-using-botulinum-toxin
- Turner-Stokes L, Jacinto J, Fheodoroff K, Brashear A, Maisonobe P, Lysandropoulos A, et al. Longitudinal goal attainment with integrated upper limb spasticity management including repeat injections of botulinum toxin A: findings from the prospective, observational Upper Limb International Spasticity (ULIS-III) cohort study. J Rehabil Med 2021; 53 (2): jrm00157. Available from: http://www.ncbi.nlm.nih.gov/pubmed/33616192
- Hamer M, Lavoie KL, Bacon SL. Taking up physical activity in later life and healthy ageing: the English longitudinal study of ageing. Br J Sports Med 2014; 48 (3): 239–243.
- Lillo N, Palomo-Vélez G, Fuentes E, Palomo I. Role of physical activity in cardiovascular disease prevention in older adults. Sport Sci Health 2015; 11 (3): 227–233.
- Saunders DH, Greig CA, Mead GE. Physical activity and exercise after stroke: review of multiple meaningful benefits. Stroke 2014; 45 (12): 3742–3747.
- Ding X-D, Zhang G-B, Chen H-X, Wang W, Song J-H, Fu D-G. Color Doppler ultrasound-guided botulinum toxin type A injection combined with an ankle foot brace for treating lower limb spasticity after a stroke. Eur Rev Med Pharmacol Sci 2015; 19 (3): 406–411. Available from: http://www.ncbi.nlm.nih.gov/pubmed/25720711
- Lam K, Lau KK, So KK, Tam CK, Wu YM, Cheung G, et al. Can botulinum toxin decrease carer burden in long term care residents with upper limb spasticity? A randomized controlled study. J Am Med Dir Assoc 2012; 13 (5): 477–84. Available from: http://dx.doi.org/10.1016/j.jamda.2012.03.005
- Doan QV, Brashear A, Gillard PJ, Varon SF, Vandenburgh AM, Turkel CC, et al. Relationship between disability and health-related quality of life and caregiver burden in patients with upper limb poststroke spasticity. PM R 2012; 4 (1): 4–10. Available from: http://dx.doi.org/10.1016/j.pmrj.2011.10.001
- Snow BJ, Tsui JKC, Bhatt MH, Varelas M, Hashimoto SA, Calne DB. Treatment of spasticity with botulinum toxin: a double-blind study. Ann Neurol 1990; 28 (4): 512–515.
- Kelly J, Rudd A, Lewis R, Hunt BJ. Venous thromboembolism after acute stroke. Stroke 2001; 32 (1): 262–267. Available from: http://www.ncbi.nlm.nih.gov/pubmed/11136946
- Gupta AD, Addison S. Healing hand ulcers caused by focal spasticity. Int Wound J 2020; 17 (3): 774–780. Available from: http://www.ncbi.nlm.nih.gov/pubmed/32135027
- Joint Formulary Committee (April 2021). British national formulary. Available from: https://bnf.nice.org.uk/
- 2018/19 National Cost Collection Data Publication. Available from: https://www.england.nhs.uk/publication/2018-19-national-cost-collection-data-publication/