Effect of inspiratory muscle training on inspiratory muscle strength in adults with post-COVID-19 condition and inspiratory muscle weakness: a randomized controlled trial
DOI:
https://doi.org/10.2340/jrm.v58.44931Keywords:
Breathing Exercises, Long COVID, Maximal Inspiratory Pressure, Minimal Clinically Important Improvement, Physical Exercise, Randomized Controlled Trial, Respiratory Muscle Training, Signs and Symptoms, RespiratoryAbstract
Objective: Evaluate the effect of inspiratory muscle training in adults with post-COVID-19 condition (PCC) and inspiratory muscle weakness.
Design: Randomized controlled trial.
Subjects/Patients: Adults with PCC and inspiratory muscle weakness.
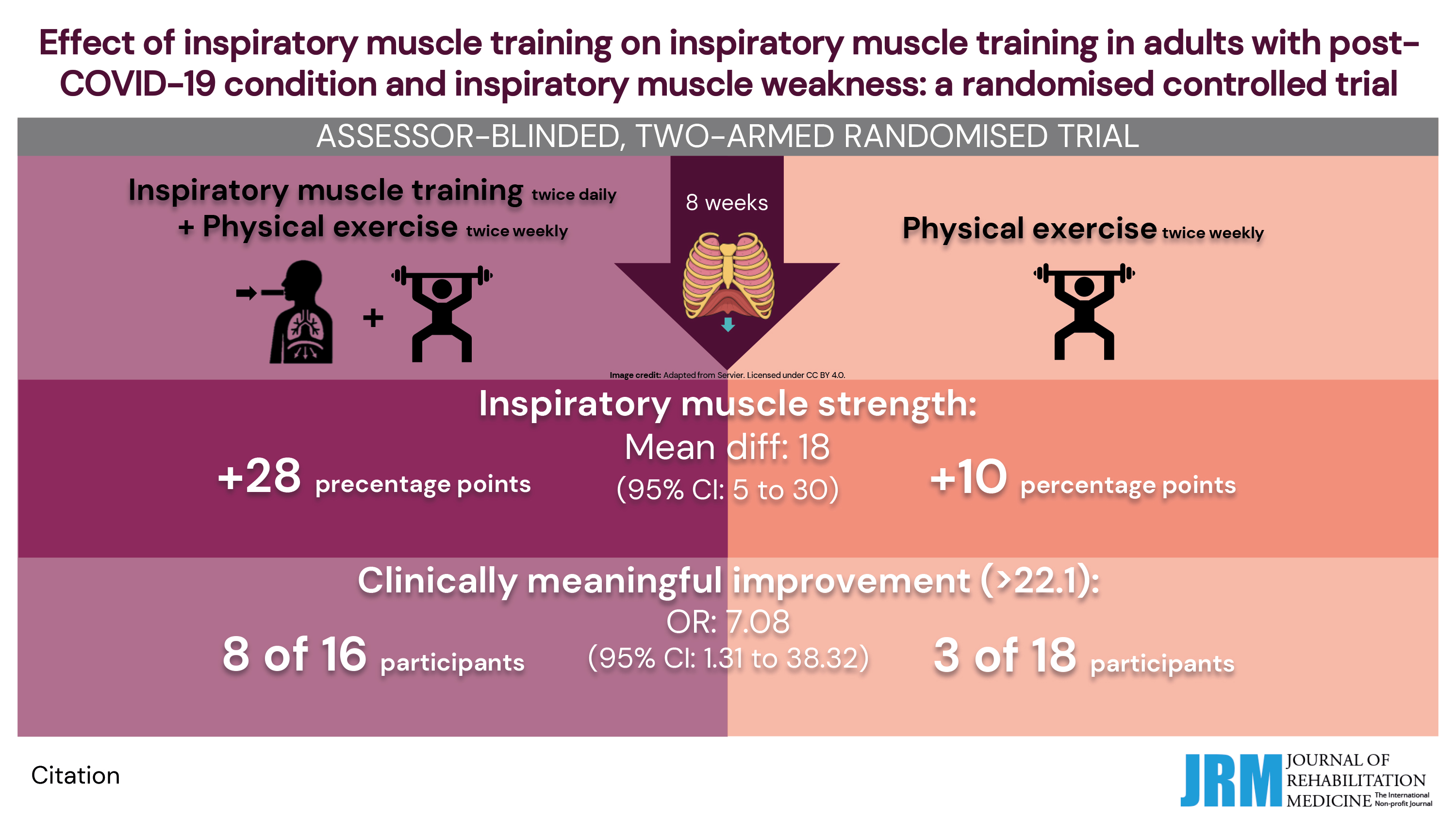
Methods: Participants were randomized to inspiratory muscle training twice daily plus individualized exercise twice weekly or exercise alone, with weekly follow-ups over 8 weeks. Primary outcome: inspiratory muscle strength (Maximal Inspiratory Pressure). Secondary outcomes: expiratory muscle strength (Maximal Expiratory Pressure); functional capacity (Six‑Minute Walk Test; One‑Minute Sit‑to‑Stand); lung function (spirometry); dyspnoea (mMRC); respiratory symptoms (chest tightness, impaired deep breathing, breathing‑related pain); cough frequency (CAAT cough item); fatigue (Fatigue Severity Scale); physical activity (Frändin–Grimby Activity Scale); activity limitations (Patient‑Specific Functional Scale); and health-related quality of life (EQ‑5D‑5L). Intention-to-treat analyses used imputed missing data. Estimated sample size: 90.
Results: Forty-four participants were included (median age 47; 82% women; n = 22/group). Between‑group differences favoured the intervention for inspiratory muscle strength (mean difference: 18%; 95% CI: 5–30; OR for clinically meaningful improvement: 7.08, 95% CI: 1.31–38.32) and cough frequency. No other between-group differences were observed.
Conclusion: Inspiratory muscle training may improve inspiratory muscle strength and reduce cough frequency, but limited sample size and underrepresentation of the most severely affected warrant cautious interpretation.
Downloads
References
Soriano JB, Murthy S, Marshall JC, Relan P, Diaz JV. A clinical case definition of post-COVID-19 condition by a Delphi consensus. Lancet Infect Dis 2022; 22: e102–e107.
https://doi.org/10.1016/S1473-3099(21)00703-9 DOI: https://doi.org/10.1016/S1473-3099(21)00703-9
Lewthwaite H, Byrne A, Brew B, Gibson PG. Treatable traits for long COVID. Respirology 2023; 28: 1005–1022.
https://doi.org/10.1111/resp.14596 DOI: https://doi.org/10.1111/resp.14596
Greenhalgh T, Sivan M, Perlowski A, Nikolich JŽ. Long COVID: a clinical update. Lancet 2024; 404: 707–724.
https://doi.org/10.1016/S0140-6736(24)01136-X DOI: https://doi.org/10.1016/S0140-6736(24)01136-X
Perola M, Nygren-Bonnier M, Søraas A, Nyborg G, Valdimarsdottír U, Øvrehus A. Knowledge development post-COVID-19: Nordic policy paper [Internet]. Oslo: NordForsk; 2025 [cited 2026 Jan 26]. Available from: https://www.nordforsk.org/2025/knowledge-development-post-covid-19
Fang Z, Ahrnsbrak R, Rekito A. Evidence mounts that about 7% of US adults have had long COVID. JAMA 2024; 332: 5–6.
https://doi.org/10.1001/jama.2024.11370 DOI: https://doi.org/10.1001/jama.2024.11370
Fagevik Olsén M, Lannefors L, Nygren-Bonnier M, Johansson E-L. Long COVID – respiratory symptoms in non-hospitalised subjects – a cross-sectional study. Eur J Physiother 2022; 24: 1–8.
https://doi.org/10.1080/21679169.2022.2101692 DOI: https://doi.org/10.1080/21679169.2022.2101692
Severin R, Franz CK, Farr E, Meirelles C, Arena R, Phillips SA, et al. The effects of COVID-19 on respiratory muscle performance: making the case for respiratory muscle testing and training. Eur Respir Rev 2022; 31.
https://doi.org/10.1183/16000617.0006-2022 DOI: https://doi.org/10.1183/16000617.0006-2022
Iqbal MM, Iqbal A, Evans RA. Long COVID update: respiratory sequelae and symptoms. Curr Opin Support Palliat Care 2025; 19: 95-102.
https://doi.org/10.1097/spc.0000000000000755 DOI: https://doi.org/10.1097/SPC.0000000000000755
Fedorowski A, Olsén MF, Nikesjö F, Janson C, Bruchfeld J, Lerm M, et al. Cardiorespiratory dysautonomia in post-COVID-19 condition: manifestations, mechanisms and management. J Intern Med 2023; 294: 548–562.
https://doi.org/10.1111/joim.13652 DOI: https://doi.org/10.1111/joim.13652
Chan JS, Mann LM, Doherty CJ, Angus SA, Thompson BP, Devries MC, et al. The effect of inspiratory muscle training and detraining on the respiratory metaboreflex. Exp Physiol 2023; 108: 636–649.
https://doi.org/10.1113/ep090779 DOI: https://doi.org/10.1113/EP090779
Spiesshoefer J, Regmi B, Senol M, Jörn B, Gorol O, Elfeturi M, et al. Potential diaphragm muscle weakness-related dyspnea persists 2 years after COVID-19 and could be improved by inspiratory muscle training: results of an observational and an interventional clinical trial. Am J Respir Crit Care Med 2024; 210: 618–628.
https://doi.org/10.1164/rccm.202309-1572OC DOI: https://doi.org/10.1164/rccm.202309-1572OC
Arienti C, Lazzarini SG, Andrenelli E, Cordani C, Negrini F, Pollini E, et al. Rehabilitation and COVID-19: systematic review by Cochrane Rehabilitation. Eur J Phys Rehabil Med 2023; 59: 800–818.
https://doi.org/10.23736/S1973-9087.23.08331-4 DOI: https://doi.org/10.23736/S1973-9087.23.08331-4
Del Corral T, Fabero-Garrido R, Plaza-Manzano G, Fernández-de-Las-Peñas C, Navarro-Santana M, López-de-Uralde-Villanueva I. Home-based respiratory muscle training on quality of life and exercise tolerance in long-term post-COVID-19: randomized controlled trial. Ann Phys Rehabil Med 2023; 66: 101709.
https://doi.org/10.1016/j.rehab.2022.101709 DOI: https://doi.org/10.1016/j.rehab.2022.101709
Jimeno-Almazán A, Buendía-Romero Á, Martínez-Cava A, Franco-López F, Sánchez-Alcaraz BJ, Courel-Ibáñez J, et al. Effects of a concurrent training, respiratory muscle exercise, and self-management recommendations on recovery from post-COVID-19 conditions: the RECOVE trial. J Appl Physiol (1985) 2023; 134: 95–104.
https://doi.org/10.1152/japplphysiol.00489.2022 DOI: https://doi.org/10.1152/japplphysiol.00489.2022
McNarry MA, Berg RMG, Shelley J, Hudson J, Saynor ZL, Duckers J, et al. Inspiratory muscle training enhances recovery post-COVID-19: a randomised controlled trial. Eur Respir J 2022; 60: 2103101.
https://doi.org/10.1183/13993003.03101-2021 DOI: https://doi.org/10.1183/13993003.03101-2021
Del Corral T, Fabero-Garrido R, Plaza-Manzano G, Izquierdo-García J, López-Sáez M, García-García R, et al. Effect of respiratory rehabilitation on quality of life in individuals with post-COVID-19 symptoms: a randomised controlled trial. Ann Phys Rehabil Med 2025; 68: 101920.
https://doi.org/10.1016/j.rehab.2024.101920 DOI: https://doi.org/10.1016/j.rehab.2024.101920
Rydwik E, Anmyr L, Regardt M, McAllister A, Zarenoe R, Åkerman E, et al. ReCOV: recovery and rehabilitation during and after COVID-19: a study protocol of a longitudinal observational study on patients, next of kin and health care staff. BMC Sports Sci Med Rehabil 2021; 13: 70.
https://doi.org/10.1186/s13102-021-00299-9 DOI: https://doi.org/10.1186/s13102-021-00299-9
Nygren-Bonnier M, Svensson-Raskh A, Holmström L, Törnberg A, Svensson A, Loewenstein D, et al. Health outcomes in hospitalised and non-hospitalised individuals after COVID-19: an observational, cross-sectional study. Commun Med 2025; 5: 512.
https://doi.org/10.1038/s43856-025-01251-5 DOI: https://doi.org/10.1038/s43856-025-01251-5
Sclauser Pessoa IM, Franco Parreira V, Fregonezi GA, Sheel AW, Chung F, Reid WD. Reference values for maximal inspiratory pressure: a systematic review. Can Respir J 2014; 21: 43–50.
https://doi.org/10.1155/2014/982374 DOI: https://doi.org/10.1155/2014/982374
Borg GA. Psychophysical bases of perceived exertion. Med Sci Sports Exerc 1982; 14: 377–381.
https://doi.org/10.1249/00005768-198205000-00012 DOI: https://doi.org/10.1249/00005768-198205000-00012
Del Corral T, Fabero-Garrido R, Plaza-Manzano G, Fernández-de-Las-Peñas C, Navarro-Santana MJ, López-de-Uralde-Villanueva I. Minimal clinically important differences in inspiratory muscle function variables after a respiratory muscle training programme in individuals with long-term post-COVID-19 symptoms. J Clin Med 2023; 12: 2720.
https://doi.org/10.3390/jcm12072720 DOI: https://doi.org/10.3390/jcm12072720
Laveneziana P, Albuquerque A, Aliverti A, Babb T, Barreiro E, Dres M, et al. ERS statement on respiratory muscle testing at rest and during exercise. Eur Respir J 2019; 53: 1801214.
https://doi.org/10.1183/13993003.01214-2018 DOI: https://doi.org/10.1183/13993003.01214-2018
American Thoracic Society. ATS statement: guidelines for the six-minute walk test. Am J Respir Crit Care Med 2002; 166: 111–117.
https://doi.org/10.1164/ajrccm.166.1.at1102 DOI: https://doi.org/10.1164/ajrccm.166.1.at1102
Enright PL, Sherrill DL. Reference equations for the six-minute walk in healthy adults. Am J Respir Crit Care Med 1998; 158: 1384–1387.
https://doi.org/10.1164/ajrccm.158.5.9710086 DOI: https://doi.org/10.1164/ajrccm.158.5.9710086
Strassmann A, Steurer-Stey C, Lana KD, Zoller M, Turk AJ, Suter P, et al. Population-based reference values for the 1-min sit-to-stand test. Int J Public Health 2013; 58: 949–953.
https://doi.org/10.1007/s00038-013-0504-z DOI: https://doi.org/10.1007/s00038-013-0504-z
Graham BL, Steenbruggen I, Miller MR, Barjaktarevic IZ, Cooper BG, Hall GL, et al. Standardization of spirometry 2019 update: an official American Thoracic Society and European Respiratory Society technical statement. Am J Respir Crit Care Med 2019; 200: e70–e88.
https://doi.org/10.1164/rccm.201908-1590ST DOI: https://doi.org/10.1164/rccm.201908-1590ST
Halpin DMG, Criner GJ, Papi A, Singh D, Anzueto A, Martinez FJ, et al. Global initiative for the diagnosis, management, and prevention of chronic obstructive lung disease. The 2020 GOLD science committee report on COVID-19 and chronic obstructive pulmonary disease. Am J Respir Crit Care Med 2021; 203: 24–36.
https://doi.org/10.1164/rccm.202009-3533SO DOI: https://doi.org/10.1164/rccm.202009-3533SO
Jones PW, Tomaszewski EL, Belton L, Burgel P-R, Hughes R, Keen C, et al. Validity of the Chronic Airways Assessment Test (CAAT) in asthma, asthma+COPD and COPD in NOVELTY. ERJ Open Res 2024; 10: 01359–2024.
https://doi.org/10.1183/23120541.01359-2024 DOI: https://doi.org/10.1183/23120541.01359-2024
Mattsson M, Möller B, Lundberg I, Gard G, Boström C. Reliability and validity of the Fatigue Severity Scale in Swedish for patients with systemic lupus erythematosus. Scand J Rheumatol 2008; 37: 269–277.
https://doi.org/10.1080/03009740801914868 DOI: https://doi.org/10.1080/03009740801914868
Grimby G, Frändin K. On the use of a six-level scale for physical activity. Scand J Med Sci Sports 2018; 28: 819–825.
https://doi.org/10.1111/sms.12991 DOI: https://doi.org/10.1111/sms.12991
Mathis RA, Taylor JD, Odom BH, Lairamore C. Reliability and validity of the Patient-Specific Functional Scale in community-dwelling older adults. J Geriatr Phys Ther 2019; 42: E67–E72.
https://doi.org/10.1519/jpt.0000000000000188 DOI: https://doi.org/10.1519/JPT.0000000000000188
Herdman M, Gudex C, Lloyd A, Janssen M, Kind P, Parkin D, et al. Development and preliminary testing of the new five-level version of EQ-5D (EQ-5D-5L). Qual Life Res 2011; 20: 1727–1736.
https://doi.org/10.1007/s11136-011-9903-x DOI: https://doi.org/10.1007/s11136-011-9903-x
Del Corral T, Fabero-Garrido R, Plaza-Manzano G, Navarro-Santana MJ, Fernández-de-Las-Peñas C, López-de-Uralde-Villanueva I. Minimal clinically important differences in EQ-5D-5L index and VAS after a respiratory muscle training program in individuals experiencing long-term post-COVID-19 symptoms. Biomedicines 2023; 11: 2522.
https://doi.org/10.3390/biomedicines11092522 DOI: https://doi.org/10.3390/biomedicines11092522
Lakens D. Calculating and reporting effect sizes to facilitate cumulative science: a practical primer for t-tests and ANOVAs. Front Psychol 2013; 4: 863.
https://doi.org/10.3389/fpsyg.2013.00863 DOI: https://doi.org/10.3389/fpsyg.2013.00863
Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG. Research electronic data capture (REDCap): a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform 2009; 42: 377–381.
https://doi.org/10.1016/j.jbi.2008.08.010 DOI: https://doi.org/10.1016/j.jbi.2008.08.010
R Core Team. R: A language and environment for statistical computing [Internet]. Vienna: R Foundation for Statistical Computing; 2024 [cited 2026 Jan 26]. Available from: https://www.R-project.org/
Vickers AJ. The use of percentage change from baseline as an outcome in a controlled trial is statistically inefficient: a simulation study. BMC Med Res Methodol 2001; 1: 6.
https://doi.org/10.1186/1471-2288-1-6 DOI: https://doi.org/10.1186/1471-2288-1-6
Shah AD, Bartlett JW, Carpenter J, Nicholas O, Hemingway H. Comparison of random forest and parametric imputation models for imputing missing data using MICE: a CALIBER study. Am J Epidemiol 2014; 179: 764–774.
https://doi.org/10.1093/aje/kwt312 DOI: https://doi.org/10.1093/aje/kwt312
World Physiotherapy. World Physiotherapy response to COVID-19 briefing paper 9: safe rehabilitation approaches for people living with long COVID: physical activity and exercise [Internet]. London: World Physiotherapy; 2021 [cited 2026 Jan 26]. Available from: https://world.physio/sites/default/files/2021-06/Briefing-Paper-9-Long-Covid-FINAL-2021.pdf
World Health Organization. Clinical management of COVID-19: living guideline [Internet]. Geneva: World Health Organization; 2023 [updated 2023 Aug 18; cited 2026 Jan 26]. Available from: https://iris.who.int/bitstream/handle/10665/372288/WHO-2019-nCoV-clinical-2023.2-eng.pdf
Downloads
Additional Files
Published
How to Cite
License
Copyright (c) 2026 Anna Törnberg, Anna Svensson-Raskh, Elisabeth Rydwik, Alexandra Halvarsson, Judith Bruchfeld, Malin Nygren-Bonnier

This work is licensed under a Creative Commons Attribution 4.0 International License.
All digitalized JRM contents is available freely online. The Foundation for Rehabilitation Medicine owns the copyright for all material published until volume 40 (2008), as from volume 41 (2009) authors retain copyright to their work and as from volume 49 (2017) the journal has been published Open Access, under CC-BY-NC licences (unless otherwise specified). The CC-BY-NC licenses allow third parties to copy and redistribute the material in any medium or format and to remix, transform, and build upon the material for non-commercial purposes, provided proper attribution to the original work.
From 2024, articles are published under the CC-BY licence. This license permits sharing, adapting, and using the material for any purpose, including commercial use, with the condition of providing full attribution to the original publication.





