Chronic Pruritus in Older Adults: Prevalence, Associations, and Pruritus-specific Quality of Life
DOI:
https://doi.org/10.2340/actadv.v105.44313Keywords:
Chronic itch, Chronic pruritus, epidemiology of itch, associated factor, Quality of life, older adultsAbstract
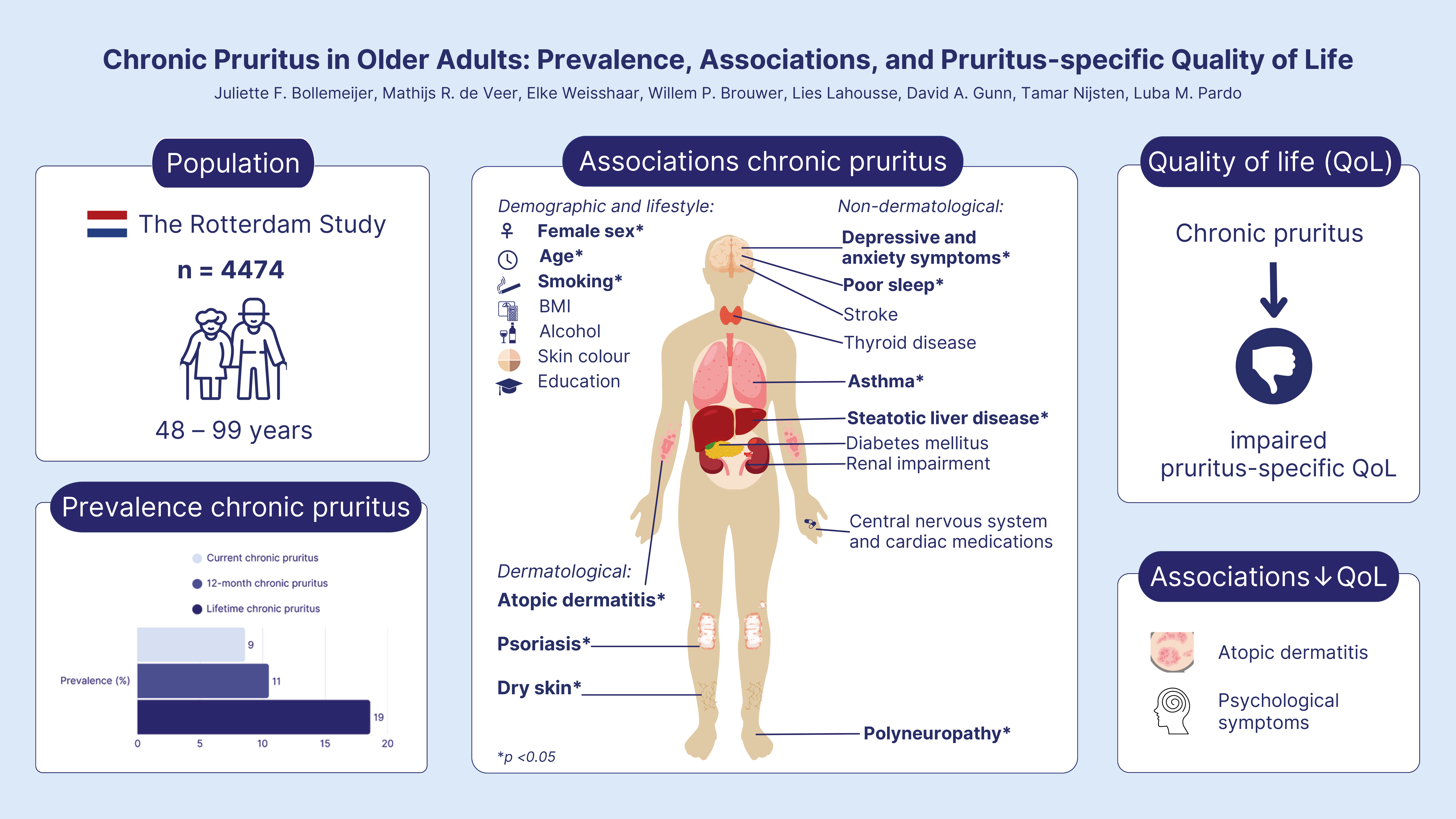
Chronic pruritus is a burdensome condition that frequently affects older adults, yet its epidemiology and impact on quality of life in the ageing population remain underexplored. This cross-sectional study examined the prevalence of chronic pruritus, its associated factors, and pruritus-specific quality of life in 4,474 participants (median age: 72 years; range: 48–99, 58.8% female) from the population-based Rotterdam Study. Questionnaires assessed current, 12-month, and lifetime chronic pruritus, along with the ItchyQoL. Multivariable logistic regression identified factors associated with chronic pruritus, and linear regression assessed factors linked to pruritus-specific quality of life. Principal component analysis explored the ItchyQoL’s dimensional structure in this older population. Chronic pruritus prevalence was 8.6% (current), 10.5% (12-month), and 18.6% (lifetime). Female sex, older age, smoking, atopic dermatitis, psoriasis, self-reported dry skin, asthma, steatotic liver disease, polyneuropathy, depressive symptoms, anxiety, and poor sleep were associated with higher odds of chronic pruritus. Among those with current chronic pruritus, pruritus-specific quality of life was moderately impaired, with the greatest impairment associated with atopic dermatitis and psychological symptoms. Principal component analysis identified 4 ItchyQoL dimensions, extending beyond the original 3 domains. Given the cross-sectional design, directionality cannot be inferred. These findings highlight chronic pruritus as a prevalent, multifactorial condition in older adults, with significant psychological impact and implications for multidisciplinary management.
Downloads
References
Yosipovitch G, Rosen JD, Hashimoto T. Itch: from mechanism to (novel) therapeutic approaches. J Allergy Clin Immunol 2018; 142: 1375–1390. DOI: https://doi.org/10.1016/j.jaci.2018.09.005
Ständer S, Schmelz M, Lerner E, Murota H, Nattkemper L, Reich A, et al. A multidisciplinary Delphi consensus on the modern definition of pruritus: sensation and disease. J Eur Acad Dermatol Venereol 2025. DOI: https://doi.org/10.1111/jdv.20851
Pereira MP, Zeidler C, Storck M, Agelopoulos K, Philipp-Dormston WG, Zink A, Ständer S. Challenges in clinical research and care in pruritus. Acta Derm Venereol 2020; 100: adv00028. DOI: https://doi.org/10.2340/00015555-3348
Kini SP, DeLong LK, Veledar E, McKenzie-Brown AM, Schaufele M, Chen SC. The impact of pruritus on quality of life: the skin equivalent of pain. Arch Dermatol 2011; 147: 1153–1156. DOI: https://doi.org/10.1001/archdermatol.2011.178
Butler DC, Berger T, Elmariah S, Kim B, Chisolm S, Kwatra SG, et al. Chronic pruritus: a review. JAMA 2024; 331: 2114–2124. DOI: https://doi.org/10.1001/jama.2024.4899
Chung BY, Um JY, Kim JC, Kang SY, Park CW, Kim HO. Pathophysiology and treatment of pruritus in elderly. Int J Mol Sci 2020; 22. DOI: https://doi.org/10.3390/ijms22010174
Reich A, Ständer S, Szepietowski JC. Pruritus in the elderly. Clin Dermatol 2011; 29: 15–23. DOI: https://doi.org/10.1016/j.clindermatol.2010.07.002
Lee J, Suh H, Jung H, Park M, Ahn J. Association between chronic pruritus, depression, and insomnia: a cross-sectional study. JAAD Int 2021; 3: 54–60. DOI: https://doi.org/10.1016/j.jdin.2021.02.004
Reszke R, Szepietowski JC. Itch and psyche: bilateral associations. Acta Derm Venereol 2020; 100: 28–36. DOI: https://doi.org/10.2340/00015555-3346
Sanders KM, Akiyama T. The vicious cycle of itch and anxiety. Neurosci Biobehav Rev 2018; 87: 17–26. DOI: https://doi.org/10.1016/j.neubiorev.2018.01.009
Ferreira BR, Katamanin OM, Jafferany M, Misery L. Psychodermatology of chronic pruritus: an overview of the link between itch and distress. Dermatol Ther (Heidelb) 2024; 14: 1799–1809. DOI: https://doi.org/10.1007/s13555-024-01214-z
Choragudi S, Biazus Soares G, Yosipovitch G. Predictive factors of quality of life in chronic pruritus patients: a cross-sectional study. JAAD Int 2023; 11: 65–71. DOI: https://doi.org/10.1016/j.jdin.2022.12.005
Lipman ZM, Yap QV, Rosen J, Nattkemper L, Yosipovitch G. The association of chronic pruritus with patients’ quality of life: a cross-sectional study. J Am Acad Dermatol 2022; 86: 448–450. DOI: https://doi.org/10.1016/j.jaad.2021.09.062
Cornman HL, Whang KA, Ma E, Aggarwal P, Kambala A, Reddy SV, et al. Severity, impact on quality of life and mental health burden of pruritus in prurigo nodularis: a cross-sectional study of a diverse patient cohort. Br J Dermatol 2024; 190: 571–572. DOI: https://doi.org/10.1093/bjd/ljad500
Carr CW, Veledar E, Chen SC. Factors mediating the impact of chronic pruritus on quality of life. JAMA Dermatol 2014; 150: 613–620. DOI: https://doi.org/10.1001/jamadermatol.2013.7696
Zeidler C, Kupfer J, Dalgard FJ, Bewley A, Evers AWM, Gieler U, et al. Dermatological patients with itch report more stress, stigmatization experience, anxiety and depression compared to patients without itch: results from a European multi-centre study. J Eur Acad Dermatol Venereol 2024; 38: 1649–1661. DOI: https://doi.org/10.1111/jdv.19913
Erickson S, Heul AV, Kim BS. New and emerging treatments for inflammatory itch. Ann Allergy Asthma Immunol 2021; 126: 13–20. DOI: https://doi.org/10.1016/j.anai.2020.05.028
Lam M, Zhu JW, Maqbool T, Adam G, Tadrous M, Rochon P, et al. Inclusion of older adults in randomized clinical trials for systemic medications for atopic dermatitis: a systematic review. JAMA Dermatol 2020; 156: 1240–1245. DOI: https://doi.org/10.1001/jamadermatol.2020.2940
Schaap MJ, van Winden MEC, Seyger MMB, de Jong E, Lubeek SFK. Representation of older adults in randomized controlled trials on systemic treatment in plaque psoriasis: a systematic review. J Am Acad Dermatol 2020; 83: 412–424. DOI: https://doi.org/10.1016/j.jaad.2019.07.079
Desai NS, Poindexter GB, Monthrope YM, Bendeck SE, Swerlick RA, Chen SC. A pilot quality-of-life instrument for pruritus. J Am Acad Dermatol 2008; 59: 234–244. DOI: https://doi.org/10.1016/j.jaad.2008.04.006
Ikram MA, Kieboom BCT, Brouwer WP, Brusselle G, Chaker L, Ghanbari M, et al. The Rotterdam Study: design update and major findings between 2020 and 2024. Eur J Epidemiol 2024; 39: 183–206. DOI: https://doi.org/10.1007/s10654-023-01094-1
Matterne U, Strassner T, Apfelbacher CJ, Diepgen TL, Weisshaar E. Measuring the prevalence of chronic itch in the general population: development and validation of a questionnaire for use in large-scale studies. Acta Derm Venereol 2009; 89: 250–256. DOI: https://doi.org/10.2340/00015555-0641
Storck M, Sandmann S, Bruland P, Pereira MP, Steinke S, Riepe C, et al. Pruritus Intensity Scales across Europe: a prospective validation study. J Eur Acad Dermatol Venereol 2021; 35: 1176–1185. DOI: https://doi.org/10.1111/jdv.17111
Bollemeijer JF, Zheng KJ, van der Meer AM, Ikram MK, Kavousi M, Brouwer WP, et al. Lifetime prevalence and associated factors of itch with skin conditions: atopic dermatitis, psoriasis and dry skin in individuals aged over 50. Clin Exp Dermatol 2024; 49: 1036–1043. DOI: https://doi.org/10.1093/ced/llae077
Williams HC, Burney PG, Pembroke AC, Hay RJ. Validation of the U.K. diagnostic criteria for atopic dermatitis in a population setting. U.K. Diagnostic Criteria for Atopic Dermatitis Working Party. Br J Dermatol 1996; 135: 12–17. DOI: https://doi.org/10.1111/j.1365-2133.1996.tb03599.x
Jacobs LC, Hamer MA, Verkouteren JA, Pardo LM, Liu F, Nijsten T. Perceived skin colour seems a swift, valid and reliable measurement. Br J Dermatol 2015; 173: 1084–1086. DOI: https://doi.org/10.1111/bjd.13888
Reich A, Ständer S, Szepietowski JC. Drug-induced pruritus: a review. Acta Derm Venereol 2009; 89: 236–244. DOI: https://doi.org/10.2340/00015555-0650
Radloff LS. The CES-D Scale: a self-report depression scale for research in the general population. Appl Psychol Meas 1977; 1: 385–401. DOI: https://doi.org/10.1177/014662167700100306
Beekman ATF, Van Limbeek J, Deeg DJH, Wouters L, Van Tilburg W. Screening for depression in the elderly in the community: using the Center for Epidemiologic Studies Depression Scale (CES-D) in the Netherlands. Tijdschrift voor Gerontologie en Geriatrie 1994; 25: 95–103 (in Dutch).
Zigmond AS, Snaith RP. The hospital anxiety and depression scale. Acta Psychiatr Scand 1983; 67: 361–370. DOI: https://doi.org/10.1111/j.1600-0447.1983.tb09716.x
Buysse DJ, Reynolds CF 3rd, Monk TH, Berman SR, Kupfer DJ. The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res 1989; 28: 193–213. DOI: https://doi.org/10.1016/0165-1781(89)90047-4
von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP, Initiative S. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet 2007; 370: 1453–1457. DOI: https://doi.org/10.1016/S0140-6736(07)61602-X
Matterne U, Apfelbacher CJ, Loerbroks A, Schwarzer T, Buttner M, Ofenloch R, et al. Prevalence, correlates and characteristics of chronic pruritus: a population-based cross-sectional study. Acta Derm Venereol 2011; 91: 674–679. DOI: https://doi.org/10.2340/00015555-1159
Chen S, Zhou F, Xiong Y. Prevalence and risk factors of senile pruritus: a systematic review and meta-analysis. BMJ Open 2022; 12: e051694. DOI: https://doi.org/10.1136/bmjopen-2021-051694
Ju Y, Pei H, Kang N, Zhang Y, Zhang C, Chen G, et al. Prevalence and potential risk factors of chronic pruritus among community middle-aged and older population in Beijing, China. J Eur Acad Dermatol Venereol 2022; 36: 1074–1079. DOI: https://doi.org/10.1111/jdv.18041
Valdes-Rodriguez R, Mollanazar NK, González-Muro J, Nattkemper L, Torres-Alvarez B, López-Esqueda FJ, et al. Itch prevalence and characteristics in a Hispanic geriatric population: a comprehensive study using a standardized itch questionnaire. Acta Derm Venereol 2015; 95: 417–421. DOI: https://doi.org/10.2340/00015555-1968
Yosipovitch G, Skayem C, Saint Aroman M, Taieb C, Inane M, Ben Hayoun Y, et al. International study on prevalence of itch: examining the role of itch as a major global public health problem. Br J Dermatol 2024; 191: 713–718. DOI: https://doi.org/10.1093/bjd/ljae260
Matterne U, Apfelbacher CJ, Vogelgsang L, Loerbroks A, Weisshaar E. Incidence and determinants of chronic pruritus: a population-based cohort study. Acta Derm Venereol 2013; 93: 532–537. DOI: https://doi.org/10.2340/00015555-1572
Kantor R, Kim A, Thyssen JP, Silverberg JI. Association of atopic dermatitis with smoking: a systematic review and meta-analysis. J Am Acad Dermatol 2016; 75: 1119–1125 e1111. DOI: https://doi.org/10.1016/j.jaad.2016.07.017
Hergesell K, Paraskevopoulou A, Opálka L, Velebný V, Vávrová K, Dolečková I. The effect of long-term cigarette smoking on selected skin barrier proteins and lipids. Sci Rep 2023; 13: 11572. DOI: https://doi.org/10.1038/s41598-023-38178-7
Saint-André V, Charbit B, Biton A, Rouilly V, Possémé C, Bertrand A, et al. Smoking changes adaptive immunity with persistent effects. Nature 2024; 626: 827–835. DOI: https://doi.org/10.1038/s41586-023-06968-8
Bollemeijer JF, Riemann S, Thio HB, Nijsten TEC, Brusselle G, Pardo LM. Chronic cough and chronic pruritus in older adults: a population-based cross-sectional study. ERJ Open Res 2025: 00364–02025. DOI: https://doi.org/10.1183/23120541.00364-2025
Elewski B, Alexis AF, Lebwohl M, Stein Gold L, Pariser D, Del Rosso J, et al. Itch: an under-recognized problem in psoriasis. J Eur Acad Dermatol Venereol 2019; 33: 1465–1476. DOI: https://doi.org/10.1111/jdv.15450
Moniaga CS, Tominaga M, Takamori K. Mechanisms and management of itch in dry skin. Acta Derm Venereol 2020; 100: adv00024. DOI: https://doi.org/10.2340/00015555-3344
Andrade LF, Haq Z, Abdi P, Diaz MJ, Levy C, Yosipovitch G. Association of liver disease and chronic pruritus: a case-control study. Liver Int 2025; 45: e16126. DOI: https://doi.org/10.1111/liv.16126
Stefaniak AA, Krajewski PK, Bednarska-Chabowska D, Bolanowski M, Mazur G, Szepietowski JC. Itch in adult population with type 2 diabetes mellitus: clinical profile, pathogenesis and disease-related burden in a cross-sectional study. Biology (Basel) 2021; 10. DOI: https://doi.org/10.3390/biology10121332
Weisshaar E, Dalgard F. Epidemiology of itch: adding to the burden of skin morbidity. Acta Derm Venereol 2009; 89: 339–350. DOI: https://doi.org/10.2340/00015555-0662
Lipman ZM, Yosipovitch G. Substance use disorders and chronic itch. J Am Acad Dermatol 2021; 84: 148–155. DOI: https://doi.org/10.1016/j.jaad.2020.08.117
Patel P, Patel K, Pandher K, Tareen RS. The role of psychiatric, analgesic, and antiepileptic medications in chronic pruritus. Cureus 2021; 13: e17260. DOI: https://doi.org/10.7759/cureus.17260
Sinikumpu SP, Jokelainen J, Tasanen K, Timonen M, Huilaja L. Association between pruritus and psychosocial well-being: a population-based study among 6,809 subjects. Acta Derm Venereol 2023; 103: adv00837. DOI: https://doi.org/10.2340/actadv.v103.2922
Dalgard FJ, Svensson A, Halvorsen JA, Gieler U, Schut C, Tomas-Aragones L, et al. Itch and mental health in dermatological patients across Europe: a cross-sectional study in 13 countries. J Invest Dermatol 2020; 140: 568–573. DOI: https://doi.org/10.1016/j.jid.2019.05.034
Knight CP, Hauser SR, Waeiss RA, Molosh AI, Johnson PL, Truitt WA, et al. The rewarding and anxiolytic properties of ethanol within the central nucleus of the amygdala: mediated by genetic background and nociceptin. J Pharmacol Exp Ther 2020; 374: 366–375. DOI: https://doi.org/10.1124/jpet.119.262097
Krause K, Kessler B, Weller K, Veidt J, Chen SC, Martus P, et al. German version of ItchyQoL: validation and initial clinical findings. Acta Derm Venereol 2013; 93: 562–568. DOI: https://doi.org/10.2340/00015555-1544
Additional Files
Published
How to Cite
Issue
Section
Categories
License
Copyright (c) 2025 Juliette F. Bollemeijer, Mathijs R. de Veer, Elke Weisshaar, Willem P. Brouwer, Lies Lahousse, David A. Gunn, Tamar E.C. Nijsten, Luba M. Pardo

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
All digitalized ActaDV contents is available freely online. The Society for Publication of Acta Dermato-Venereologica owns the copyright for all material published until volume 88 (2008) and as from volume 89 (2009) the journal has been published fully Open Access, meaning the authors retain copyright to their work.
Unless otherwise specified, all Open Access articles are published under CC-BY-NC licences, allowing third parties to copy and redistribute the material in any medium or format and to remix, transform, and build upon the material for non-commercial purposes, provided proper attribution to the original work.





