Cutaneous Leishmaniasis in Patients under Biologic Therapies: A Spanish CLINI-AEDV Multicentre Study
DOI:
https://doi.org/10.2340/actadv.v106.adv-2025-0132Keywords:
leishmaniasis, parasitic, biological therapies, immunosuppression, TNFα antagonist, opportunistic infectionAbstract
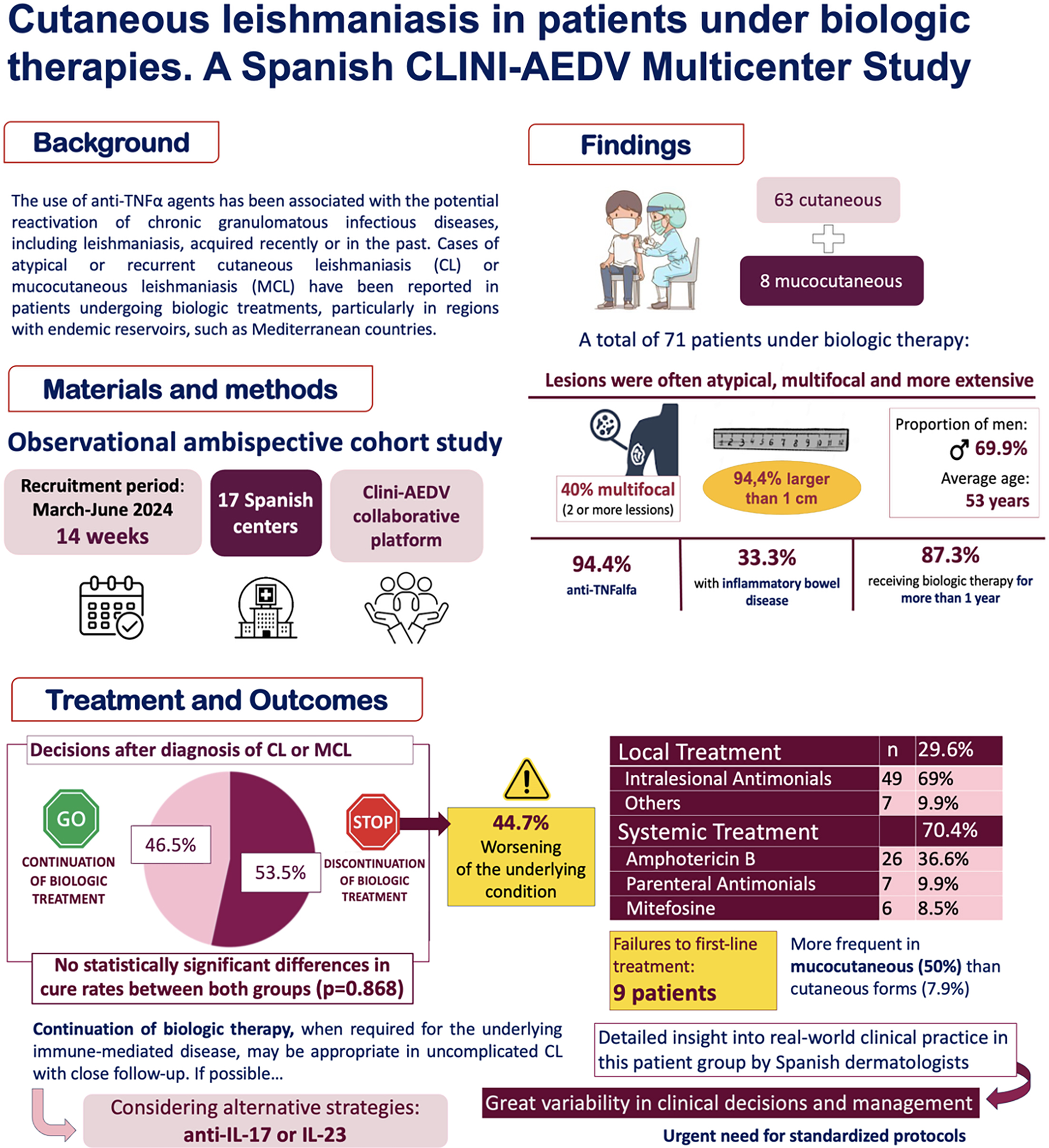
Anti-TNFα agents have been associated with the reactivation of granulomatous infections, including leishmaniasis. Cases of atypical or recurrent cutaneous (CL) or mucocutaneous leishmaniasis (MCL) have been reported in patients on biologics. We conducted a retrospective analysis of a multicenter database to describe the clinical characteristics and management of CL and MCL in patients receiving biological therapy in an endemic area. Clinical features, diagnostics, therapies, and outcomes were analyzed. Seventy-one patients were included (63 CL and 8 MCL). The most common underlying condition was inflammatory bowel disease (33.8%). Lesions were multifocal in 40% and larger than 1 cm in 94.4%. Treatment failures were more frequent in MCL (50%) than CL (8.1%). Biologic therapy was discontinued in 53.5%, leading to worsening of the underlying disease in 44.7%. No significant difference in cure rates was observed between patients who continued vs. discontinued biologics (p=0.868). These findings highlight the clinical burden of CL and MCL in patients undergoing anti-TNFα therapy and suggest that discontinuation of biologic therapy did not significantly impact cure rates, emphasizing the need for standardized strategies balancing infection control and underlying inflammatory disease management.
Downloads
References
Handler MZ, Patel PA, Kapila R, Al-Qubati Y, Schwartz RA. Cutaneous and mucocutaneous leishmaniasis: Clinical perspectives. J Am Acad Dermatol 2015; 73: 897–908. DOI: https://doi.org/10.1016/j.jaad.2014.08.051
Di Muccio T, Scalone A, Bruno A, Marangi M, Grande R, Armignacco O, et al. Epidemiology of imported leishmaniasis in Italy: implications for a European endemic country. PLoS One 2015; 10: e0129418. DOI: https://doi.org/10.1371/journal.pone.0129418
Foroutan M, Dalvand S, Khademvatan S, Majidiani H, Khalkhali H, Masoumifard S, et al. A systematic review and metaanalysis of the prevalence of Leishmania infection in blood donors. Transfus Apher Sci 2017; 56: 544–551. DOI: https://doi.org/10.1016/j.transci.2017.07.001
Maspi N, Abdoli A, Ghaffarifar F. Pro- and anti-inflammatory cytokines in cutaneous leishmaniasis: a review. Pathog Glob Health 2016; 110: 247–260. DOI: https://doi.org/10.1080/20477724.2016.1232042
Kaye P, Scott P. Leishmaniasis: complexity at the hostpathogen interface. Nat Rev Microbiol 2011; 9: 604–615. DOI: https://doi.org/10.1038/nrmicro2608
Liew FY, Parkinson C, Millott S, Severn A, Carrier M. Tumour necrosis factor (TNF alpha) in leishmaniasis. I. TNF alpha mediates host protection against cutaneous leishmaniasis. Immunology 1990; 69: 570–573.
Nascimento MSL, Carregaro V, Lima-Júnior DS, Costa DL, Ryffel B, Duthie MS, et al. Interleukin 17A acts synergistically with interferon γ to promote protection against Leishmania infantum infection. J Infect Dis 2015; 211: 1015–1026. DOI: https://doi.org/10.1093/infdis/jiu531
Palacios-Diaz RD, Sahuquillo-Torralba A, Rocamora-Durán V, Unamuno-Bustos B de, Salavert-Lleti M, Santos-Alarcón S, et al. Clinicopathological characteristics of cutaneous and mucocutaneous leishmaniasis in patients treated with TNF-α inhibitors. J Dtsch Dermatol Ges 2023; 21: 473–480. DOI: https://doi.org/10.1111/ddg.15007
Guedes-Barbosa LS, Pereira da Costa I, Fernandes V, Henrique da Mota LM, de Menezes I, Aaron Scheinberg M. Leishmaniasis during anti-tumor necrosis factor therapy: report of 4 cases and review of the literature (additional 28 cases). Semin Arthritis Rheum 2013; 43: 152–157. DOI: https://doi.org/10.1016/j.semarthrit.2013.01.006
Bosch-Nicolau P, Ubals M, Salvador F, Sánchez-Montalvá A, Aparicio G, Erra A, et al. Leishmaniasis and tumor necrosis factor alpha antagonists in the Mediterranean basin. A switch in clinical expression. PLoS Negl Trop Dis 2019; 13: e0007708. DOI: https://doi.org/10.1371/journal.pntd.0007708
Schneider P, Bouaziz JD, Foulet F, Duong TA, Allanore LV, Bagot M. Multifocal cutaneous leishmaniasis due to Leishmania infantum under adalimumab therapy. Ann Dermatol Venereol 2009; 136: 815–816. DOI: https://doi.org/10.1016/j.annder.2009.05.008
Neumayr ALC, Morizot G, Visser LG, Lockwood DNJ, Beck BR, Schneider S, et al. Clinical aspects and management of cutaneous leishmaniasis in rheumatoid patients treated with TNF-α antagonists. Travel Med Infect Dis 2013; 11: 412–420. DOI: https://doi.org/10.1016/j.tmaid.2013.05.003
Pérez-Sola MJ, Torre-Cisneros J, Pérez-Zafrilla B, Carmona L, Descalzo MA, Gómez-Reino JJ. Infections in patients treated with tumor necrosis factor antagonists: incidence, etiology and mortality in the BIOBADASER registry. Medicina Clínica 2011; 137: 533–540. DOI: https://doi.org/10.1016/j.medcli.2010.11.032
Zanger P, Kötter I, Kremsner PG, Gabrysch S. Tumor necrosis factor alpha antagonist drugs and leishmaniasis in Europe. Clin Microbiol Infect 2012; 18: 670–676. DOI: https://doi.org/10.1111/j.1469-0691.2011.03674.x
Madero-Velázquez L, Mínguez A, Mayorga L, Ramírez JJ, Moreno N, Amorós C, et al. Leishmaniasis in patients with inflammatory bowel disease: a national multicenter study of GETECCU. United European Gastroenterol J 2025; 13: 674–684. DOI: https://doi.org/10.1002/ueg2.12740
Aguado M, Espinosa P, Romero-Maté A, Tardío JC, Córdoba S, Borbujo J. Outbreak of cutaneous leishmaniasis in Fuenlabrada, Madrid. Actas Dermosifiliogr 2013; 104: 334–342. DOI: https://doi.org/10.1016/j.adengl.2013.03.005
Academia española de Dermatología y Venereología. CLINIAED case series collection platform. 2024. Available from: https://redcap.fundacionpielsana.es/surveys/?s= PKLPEJRT4XY4RKKR
Colomba C, Saporito L, Bonura S, Campisi G, Di Carlo P, Panzarella V, et al. Leishmania infection in psoriasis. Journal of Infection 2020; 80: 578–606. DOI: https://doi.org/10.1016/j.jinf.2020.01.019
De Leonardis F, Govoni M, Lo Monaco A, Trotta F. Visceral leishmaniasis and anti-TNF-alpha therapy: case report and review of the literature. Clin Exp Rheumatol 2009; 27: 503–506.
Xynos ID, Tektonidou MG, Pikazis D, Sipsas NV. Leishmaniasis, autoimmune rheumatic disease, and anti-tumor necrosis factor therapy, Europe. Emerg Infect Dis 2009; 15: 956–959. DOI: https://doi.org/10.3201/eid1506.090101
Marcoval J, Penín RM. Evolution of cutaneous leishmaniasis in the last 30 years in a tertiary hospital of the European Mediterranean coast. Int J Dermatology 2017; 56: 750–753. DOI: https://doi.org/10.1111/ijd.13588
Herrador Z, Gherasim A, Jimenez BC, Granados M del sol, San Martín JV, Aparicio P. Epidemiological changes in leishmaniasis in Spain according to hospitalization-based records, 1997-2011: raising awareness towards leishmaniasis in non- HIV patients. PLoS Negl Trop Dis 2015; 9: e0003594. DOI: https://doi.org/10.1371/journal.pntd.0003594
Daudén E, García C, Zarco C, López S, Iglesias L. Cutaneous leishmaniasis: 20 years’ experience in a Spanish tertiary care hospital. Actas Dermosifiliogr 1990; 81: 395–404.
Urrutia S, García C, Schoendorff C, Sáez A, Olivares M, García Almagro D. Cutaneous leishmaniasis in the Toledo province. A study of 43 patients. Actas Dermosifiliogr 2000; 91: 1–8.
Torres T, Chiricozzi A, Puig L, Lé AM, Marzano AV, Dapavo P, et al. Treatment of psoriasis patients with latent tuberculosis using IL-17 and IL-23 inhibitors: a retrospective, multinational, multicentre study. Am J Clin Dermatol 2024; 25: 333–342. DOI: https://doi.org/10.1007/s40257-024-00845-4
Garrido-Jareño M, Sahuquillo-Torralba A, Chouman-Arcas R, Castro-Hernández I, Molina-Moreno JM, Llavador-Ros M, et al. Cutaneous and mucocutaneous leishmaniasis: experience of a Mediterranean hospital. Parasit Vectors 2020; 13: 24. DOI: https://doi.org/10.1186/s13071-020-3901-1
Chaudhary RG, Bilimoria FE, Katare SK. Diffuse cutaneous leishmaniasis: co-infection with human immunodeficiency virus (HIV). Indian J Dermatol Venereol Leprol 2008; 74: 641–643. DOI: https://doi.org/10.4103/0378-6323.45111
Giavedoni P, Iranzo P, Fuertes I, Estrach T, Alsina Gibert M. Cutaneous leishmaniasis: 20 years’ experience in a Spanish tertiary care hospital. Actas Dermosifiliogr 2015; 106: 310–316. DOI: https://doi.org/10.1016/j.adengl.2015.03.005
Buffet PA, Rosenthal É, Gangneux JP, Lightburne E, Couppié P, Morizot G, et al. Therapy of leishmaniasis in France: consensus on proposed guidelines. Presse Med 2011; 40: 173–184. DOI: https://doi.org/10.1016/j.lpm.2010.09.023
Additional Files
Published
How to Cite
License

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
All digitalized ActaDV contents is available freely online. The Society for Publication of Acta Dermato-Venereologica owns the copyright for all material published until volume 88 (2008) and as from volume 89 (2009) the journal has been published fully Open Access, meaning the authors retain copyright to their work.
Unless otherwise specified, all Open Access articles are published under CC-BY-NC licences, allowing third parties to copy and redistribute the material in any medium or format and to remix, transform, and build upon the material for non-commercial purposes, provided proper attribution to the original work.





